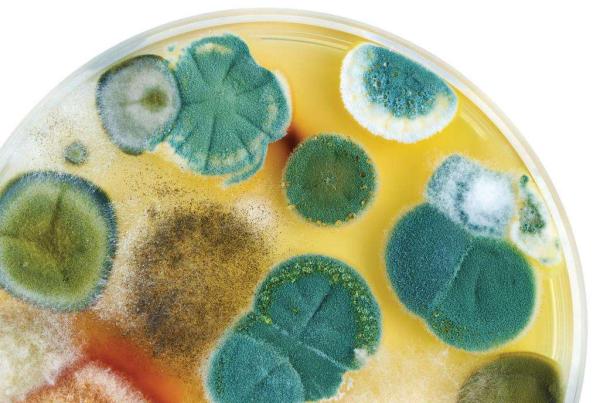
Fighting the Fungus Among Us
Overactive Immune Response Sets Stage for Infection
Fungal infections are a serious medical threat to many people, especially those who are critically ill or have weakened immune systems. What’s more, outbreaks are on the rise, as studies show that rising global temperatures are causing fungi to evolve into new strains and grow in regions that were once too cold for comfort. Recent outbreaks include a tragic incident at a Michigan paper mill that sickened nearly 100 people and caused one death, as well as a cluster of fungal infections that have killed at least seven women who underwent cosmetic surgery at clinics in Mexico.
Commemorating Fungal Disease Awareness Week this week brings attention to the importance of combating fungal threats to our well-being. The theme this year is ‘Think Fungus,’ and that’s exactly what IRP senior investigator Michail Lionakis, M.D., Sc.D., has been doing for the last 20 years.