Rare Genetic Variants Underlie Susceptibility to Reproductive Disruption
IRP Study Could Help Identify Women at Greater Risk for Fertility Problems
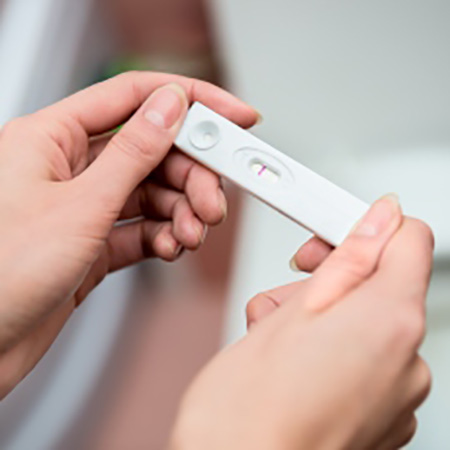
A new IRP study suggests that genetic variations influence individual susceptibility to hypothalamic amenorrhea, a condition that can halt menstrual cycles and prevent women from getting pregnant.
As the calendar page turned from 2020 to 2021, many people adopted major lifestyle changes like healthier eating or significantly increasing their physical activity. While these New Year’s resolutions will likely improve their overall health, they could also wreak havoc on the reproductive cycles of a small set of women. New IRP research sheds light on the genetic factors that make some women susceptible to diet- or exercise-induced disruptions to their reproductive systems.1
There are many reasons a woman’s period might stop occurring, a state called amenorrhea. Sometimes it is expected, as in pregnancy or menopause, but sometimes it occurs due to a rare condition called isolated hypogonadotropic hypogonadism (IHH), in which the hormonal cascade that regulates the mature reproductive system does not switch on at puberty for reasons unconnected to lifestyle factors. In other cases, dramatic shifts in a person’s exercise or eating habits can cause hypothalamic amenorrhea (HA), in which those new behaviors stress the body enough to cause the brain’s hypothalamus to stop releasing the hormones needed to maintain normal menstrual cycles.
HA is usually reversible, but for some women it can last for years or even decades, during which time they lose bone density and are unable to get pregnant. While HA is thought to affect roughly five percent of women in the general population, this rate can reach as high as 50 percent in those who exercise or reduce their food consumption. Moreover, there is dramatic variation among women in the body’s response to changes in energy intake or expenditure.

Some women can exercise heavily without developing reproductive problems, while others find that their menstrual cycles are easily thrown out of whack by changes to their diets or physical activity.
“As I started to see patients, I noticed there would be some women who could do anything — exercise however much they wanted — and their menstrual cycles would be totally normal, but then there were others for whom even small changes caused amenorrhea,” says Janet Hall, M.D., M.S., Clinical Director at the NIH’s National Institute of Environmental Health Sciences (NIEHS) and the new study’s senior author. “And that’s true on the other end as well. There were some patients concerned about their fertility where it didn’t take much for their cycles to come back, and there were others for whom, no matter what they did, it just didn’t happen.”
As a result of her observations, Dr. Hall began to suspect that genetic factors might make some women more susceptible than others to developing HA when their eating or exercise habits change. Very little research has been done on the genetics of HA, but much more is known about the genes that play a role in IHH. Since the two conditions have similar effects on the reproductive system, Dr. Hall’s team set out to compare the frequency of genetic variations in 53 IHH-related genes in women with HA and women without reproductive problems. To assist in this effort, Dr. Hall's lab teamed up with colleagues at the National Human Genome Research Institute (NHGRI) led by IRP senior investigator Joan Bailey-Wilson, Ph.D., and IRP Distinguished Investigator Leslie Biesecker, M.D.

More From the IRP
Research In Action
A Broken Link in the Chain
The study focused specifically on so-called ‘rare sequence variants’ (RSVs), which are genetic changes found in less than one percent of the general population. The IRP researchers further honed their search by looking only at variants that they deemed likely to change the way a gene produces a protein — either by changing the protein’s length or altering its chemical makeup. About 55 percent of the women with HA in the study had at least one of these rare genetic variants in an IHH-related gene, compared to only 42 percent of the women in the control group. Moreover, among the women with HA, an average of 37 percent of the genes the study examined contained a rare variant, but only 27 percent of those genes had a rare variant in the healthy women.

Photo courtesy of Steve McCaw
Dr. Janet Hall, the new study’s senior author.
“What we have shown is that there are some individuals with hypothalamic amenorrhea who have genetic variants that conceivably make them more susceptible to factors that can interfere with the reproductive system,” Dr. Hall explains.
In addition, the study found rare variants in certain genes much more often in the women with HA than the healthy women, suggesting that those genes might have a particularly large influence on risk for the condition. That observation could set the stage for future efforts to develop genetic panels that might inform the way doctors counsel patients whose periods have stopped, as well as women who want to pursue lifestyle changes that, when combined with their genetic susceptibility, could trigger HA.
“For women with fertility problems due to hypothalamic amenorrhea, this information could help to set expectations,” Dr. Hall says. “I would initially advise a change to their exercise or eating habits, but if that doesn’t work in a short period of time, I would be able to look at the patient’s genetic profile. If I see that she may be genetically more susceptible to maintaining amenorrhea even if she’s doing what she should be doing, I would move on to give her extra treatment to help her conceive.”
Subscribe to our weekly newsletter to stay up-to-date on the latest breakthroughs in the NIH Intramural Research Program.
References:
[1] Increased Burden of Rare Sequence Variants in GnRH-Associated Genes in Women with Hypothalamic Amenorrhea. Delaney A, Burkholder AM, Lavender CA, Plummer L, Merica V, Merino PM, Quinton R, Lewis KL, Meader BN, Albano A, Shaw ND, Welt CK, Martin KA, Seminara SB, Biesecker LG, Bailey-Wilson JE, Hall JE. J Clin Endocrinol Metab. 2020 Sep 1;dgaa609. doi: 10.1210/clinem/dgaa609.
Related Blog Posts
This page was last updated on Wednesday, May 24, 2023
