Closing in on the Circuitry of Chronic Itch
Genetic Studies Illuminate Neuronal Chemical’s Role in Pain and Itch
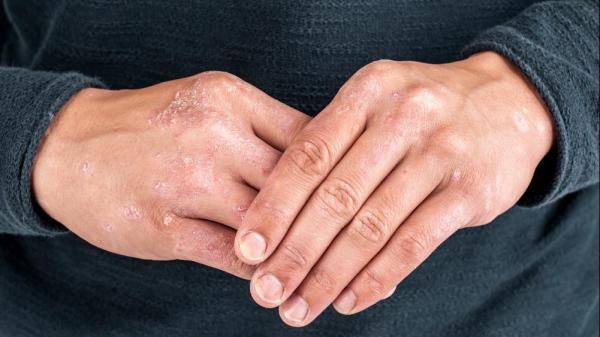
IRP research on the neurons that play a role in pain and itch could lead to treatments for numerous skin conditions, including the scaly rashes produced by psoriasis.
For most of us, itch is a bothersome inconvenience. Unfortunately, for 125 million people around the world, chronic itch caused by the skin disease psoriasis is a significant, even debilitating, health problem. Psoriasis causes skin cells to multiply up to 10 times faster than normal and build up as an itchy and painful, scaly rash. For some, the condition can also cause joint swelling, resulting in a condition known as ‘psoriatic arthritis.’
World Psoriasis Day falls on October 29 this year, and the theme is “Be Informed.” So, what do we know about chronic itch?
The mechanisms by which itch, and its cousin pain, are transmitted from the skin through the spinal cord and up to the brain are not well understood. We know that itchy sensations — whether they’re caused by a mosquito bite or a chronic disorder — are detected by sensory neurons that run through the skin. A signal lets our brain know there’s a problem, and the brain answers, “scratch!”
Evolutionarily speaking, itch is a good thing. It tells us when we’ve been exposed to something harmful like a parasite or a toxin and compels us to remove the offending critter or substance. On the other hand, chronic skin conditions like psoriasis are not so useful. Scratching damages the skin and can produce chemicals that cause the itchy sensation to increase, setting up a cycle of itching and scratching that prevents the skin from actually healing. Many treatments, such as topical creams and antihistamines, provide only moderate relief.
IRP researchers, led by Mark A. Hoon, Ph.D., are using traditional techniques and cutting-edge genetic studies to better understand this communication pathway. Back in 2018, this work led to the discovery of a new circuit in the spinal cord in which neurons release a hormone called somatostatin that can promote the sensation of itch and inhibit the feeling of pain.1 Studying this newly discovered system could lead to possible treatment targets for chronic itch.
Dr. Hoon’s team became interested in somatostatin because it showed up unexpectedly in a signaling pathway that was thought to activate itch sensation, not suppress it. It seemed paradoxical, in a system that is supposed to bring on the feeling of itch, to find an inhibitory molecule like somatostatin in a set of excitatory neurons that stimulate rather than decrease the activity of their neuronal neighbors.

Image credit: Ulrich von Andrian, M.D., Ph.D., Harvard Medical School
Neurons (red) in mouse skin communicate with dermal dendritic cells (green), a type of immune cell, to drive inflammation in psoriasis.
“It was really curious because somatostatin was in the neurons that we know are involved in itch,” says Dr. Hoon. “We were all curious what it might be doing and how it might be working.”
The answer, they found, was a compound effect. Somatostatin is an inhibitory molecule, but it reduces the activity of neurons that are also inhibitory, so the net effect is positive. In other words, it stops other neurons from blocking the sensation of itch.
To map the circuit and uncover what was happening, Dr. Hoon’s lab used a variety of techniques to stimulate itching and scratching behaviors in mice in the presence and absence of somatostatin. First, the team used a technique called optogenetics, which uses light to activate or inhibit neurons, to show that certain sensory neurons that connect to mouse skin use somatostatin to trigger itch, as evidenced by scratching behavior. The researchers also identified the cells that somatostatin inhibits to bring on itching, called dynorphin cells. Additionally, they used mice bred to lack somatostatin in their sensory neurons to show that, without somatostatin, exposure to something itchy failed to cause them to scratch. Finally, they found that somatostatin released from ‘peripheral’ neurons located outside the brain and spinal cord, but not those in the spinal cord, played a role in suppressing pain from heat.
Unfortunately, these findings on their own are not enough to suggest a solution for treating chronic itch. Somatostatin is found throughout the nervous system, so any therapeutic that blocks its effects would have significant side effects. However, understanding how somatostatin works and the neuronal circuit in which it plays its role may have implications for other ways to interrupt the itch system by targeting something along that route.
“One of the benefits of having multiple targets is that you can use them simultaneously,” Dr. Hoon explains. “That has the advantage that you can use lower doses of drugs, at levels that would normally be ineffective on their own, in combination to have an effect.”

Dr. Mark Hoon
This basic research is leading to other questions — and other findings. As part of its work, Dr. Hoon’s team has since identified other inhibitory neurons, including a variety that may play a bigger role in sensing pain. Another recent set of experiments by Dr. Hoon’s group, looked at other targets of somatostatin-releasing neurons that may be involved in producing chronic conditions like psoriasis and atopic dermatitis.
“The neurons actually changed from the normal situation and normal skin,” says Dr. Hoon. “We've identified what we think is a process by which there is this change in the sensitivity of the neurons, so it takes less input for them to start to send signals and to stimulate the parts of the brain that instruct us to scratch.”
Importantly, Dr. Hoon’s efforts could lay the groundwork for identifying solutions for chronic itch that is triggered by an abnormal immune response to skin damage rather than the itch-inducing histamine molecules that are blocked by anti-histamine medications. Such discoveries could lead to treatments for people whose chronic itch does not respond to antihistamines. However, as Dr. Hoon has discovered, the system that produces sensations of itch is complex, so his team must continue scrutinizing the nervous system to learn how best to influence it.
“The spinal cord is still a virgin forest,” says Dr. Hoon. “We’re going in there and finding new plants and animals and we don’t know exactly how they’re all interrelated with each other and how it all works. It’s exciting.”
Subscribe to our weekly newsletter to stay up-to-date on the latest breakthroughs in the NIH Intramural Research Program.
References:
[1] Circuit dissection of the role of somatostatin in itch and pain. Huang J, Polgár E, Solinski HJ, Mishra SK, Tseng PY, Iwagaki N, Boyle KA, Dickie AC, Kriegbaum MC, Wildner H, Zeilhofer HU, Watanabe M, Riddell JS, Todd AJ, Hoon MA. Nat Neurosci. 2018 May; 21(5): 707-716. doi: 10.1038/s41593-018-0119-z.
Related Blog Posts
This page was last updated on Tuesday, January 30, 2024
