Shedding Light on the Deep Darkness of Depression
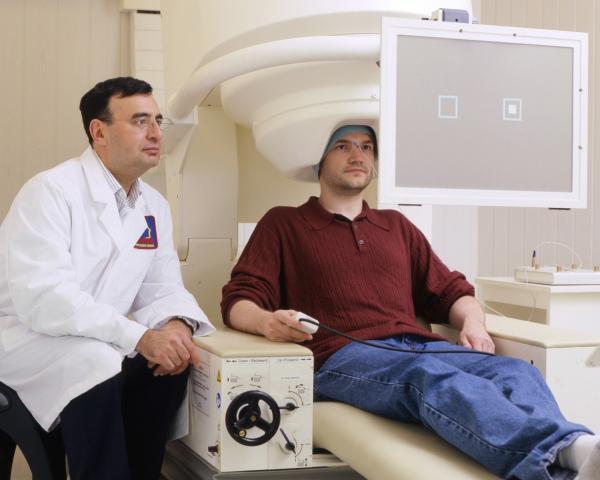
IRP senior investigator Dr. Carlos Zarate uses neuroimaging and other scientific techniques to learn about how depression affects the brain and develop more effective and rapid-acting treatments.
In 2016, more than one in twenty American adults and one in ten adolescents experienced at least one major depressive episode. For nearly 45,000 of these individuals, their condition was severe enough that it led them to take their own lives. Unfortunately, the medications currently available to treat depression are not always effective and can take up to six weeks to substantially reduce symptoms.
To improve treatment and accelerate symptom relief, IRP senior investigator Carlos Zarate Jr., M.D., is working towards the development of new medications for depression, along with the identification of new drug targets and objective measures called biomarkers that yield information about how a patient is responding to treatment. In recent years, his lab has extensively investigated and assessed the effects of the anesthetic drug ketamine on depression and suicidal thoughts. Many of the patients in his trials have had marked and rapid responses to ketamine, sometimes within a single day or just a couple of hours.
On Tuesday, November 13, Dr. Zarate participated in a Reddit “Ask Me Anything” (AMA) to answer questions from the public about the way depression is currently treated and the latest efforts to develop cutting-edge therapies for the condition. Read on for some of the most interesting exchanges that took place or check out the full AMA on Reddit.
Question (Q): “Are there any theories as to why some cases of depression are so treatment-resistant?”
Carlos Zarate, M.D.: “Current theories suggest that severe, treatment-resistant or chronic depression is not simply the result of disturbances of serotonin and norepinephrine systems but involves alterations in the resiliency and neuroplasticity of synapses and circuits. So future treatments will also need to enhance the plasticity of synapses and circuits.”
Q: “As you mentioned, many of the most frequently prescribed medications take up to six weeks to become fully effective, which can be extremely frustrating for patients (particularly if the medication ends up not working and the process starts over again). In this time between initiating a new therapy and starting to see benefits of the medication, it doesn't appear that there are many options for alleviating symptoms. Do you see something like ketamine being effective as a short-term therapy to help with symptom management during that six-week period?”
Dr. Zarate: “There is now considerable research and progress in developing treatments with a rapid onset of action — with effects in hours instead of weeks or longer. Ketamine is one example, but its side effects and potential for abuse present challenges to the clinician’s ability to use it routinely. Instead, it is reserved for the more severely ill. Investigators are exploring the use of ketamine to ‘jump start’ existing antidepressants to minimize the lag of onset of therapeutic effects. Safer forms of ketamine-like drugs are being explored. If they prove to be safe and effective, it would permit us to use them earlier in the course of treatment.”
Q: “How does ketamine work in the brain to treat depression, and what is experienced during treatment? Are the mechanisms and experiences the same or similar to other treatments currently in clinical trials for depression and PTSD, such as MDMA-assisted psychotherapy and psilocybin?”
Dr. Zarate: “There are several theories on the mechanism of how ketamine might work as an antidepressant. One theory suggests that ketamine works by blocking the NMDA glutamate receptor. Another theory suggests that changes in proteins within the cell following activation of a different sort of glutamate receptor, the AMPA receptor, are responsible for ketamine’s effects. It seems that regardless of the theory, they all converge on an increase in synaptic and circuit homeostasis, which are believed to be disrupted in depression. And as I wrote in response to another question, depression is believed to result from impairments in cellular resiliency and plasticity.
“During the infusion of ketamine given for treatment-resistant depression, patients might experience sensory disturbances, psychological symptoms (loss of awareness of surroundings, distortion of time, etc.), and increases in blood pressure and heart rate. These symptoms are time-limited and usually end shortly after the infusion of ketamine ends. Although ketamine causes hallucinogenic symptoms, the quality and nature of these are distinct from individuals who take psilocybin, LSD, MDMA, or other types of hallucinogens.”
Q: “Have you ever experienced difficulties when trying to research how recreational drugs, like ketamine or MDMA, could be used to treat conditions like depression, i.e. due to them being illegal? Similarly, how does it work legally when you are researching with illegal drugs?”
Dr. Zarate: "Research into recreational drugs is quite challenging for a number of reasons. It is possible to do such research under certain conditions and approvals. First of all, it needs to be established that there is a critical need for such research. There should be clear hypotheses and goals. Next, the drug should be studied under certain conditions. For example, when we began ketamine research in the early 2000s we made sure we addressed all regulatory approvals and ethical concerns. We also studied only individuals in our inpatient research unit, which assured close monitoring of our participants to address any potential issues that might arise. Future studies into other classes of drugs such as the hallucinogens should also consider implementing similar approaches as we did for ketamine.”
Q: “Can you please identify [a] few biomarkers that are being studied for identification of depression?”
Dr. Zarate: “Yes, there are a number of biomarkers that are being explored for depression. Some of them involve oxidative stress factors and inflammatory markers. These have harmful effects on body systems. We use blood panels to examine these as well as brain imaging. One example of imaging for these inflammatory markers is with positron emission tomography (PET) imaging looking at a protein called translocator protein, or TSPO, because amounts of TSPO in the brain are related to how much inflammation there is in the brain.”
Q: “Why do publicly available treatments seem to lag decades behind research? Why do drug companies continue to release slightly tweaked versions of SSRIs [selective serotonin reuptake inhibitors] and neglect to fund trials on novel treatments even though the medical community acknowledges the current psychiatric armamentarium is ineffective for a large portion of depressed patients?”
Dr. Zarate: “There are currently considerable efforts in developing next-generation treatments that are more robust and act more rapidly than existing treatments. These improved treatments will result from both basic and clinical research. Important insights have been obtained. Next-generation treatments will also work rapidly in other symptom domains such as suicide, PTSD symptoms, anxiety, etc. The reason for a delay in bringing drugs to market is that research usually starts with basic science studies before reaching the clinic.”
Q: “Why is there over-focus on serotonin rather than the myriad of other pathways we know that are involved in depression?”
Dr. Zarate: “Many other targets, besides serotonin, have been and continue to be pursued. Some of these targets, predominantly involving the glutamatergic system, are currently in Phase 2 and 3 clinical studies. Serotonin-type drugs dominate the market because they were the first approved for the treatment of depression and newer versions were slight improvements over existing treatments. We agree that there is a tremendous need to develop treatments that target other neurotransmitter systems that are robustly different than existing options in terms of efficacy.”
Q: “Psychiatric drugs are prone to tolerance, [and] they can stop being effective after a short time. This often requires patients to rotate therapies constantly so they never achieve an extended period of remission or receive diminishing returns with pharmacological therapy altogether. Is there any work being done on therapeutics which are less susceptible to the effects of physiological tolerance?”
Dr. Zarate: “There is some evidence that tachyphylaxis or ‘poop out syndrome’ may occur with certain treatments (i.e., they lose efficacy, which usually cannot be regained by increasing the dose). Although practitioners have tried strategies to recapture a treatment's efficacy, there has not been much systematic research into this area. Some believe that missing a couple of doses of medications or not taking medications consistently may increase the risk for tachyphylaxis.”
Q: “What properties will future medications hope to possess? Will they be immune modulatory like microglia inhibitors, potassium channel openers, dopaminergic or GABA/glutamate focused drugs?”
Dr. Zarate: “Research is moving to identify biological markers that may help ‘classify’ which type of depression one might have. For example, anti-inflammatory drugs might not help in depression as a group, but if we identify depressions that are predominantly ‘inflammatory,’ then anti-inflammatory-type drugs might help for that specific subgroup of depression. This is what is being referred to as personalized medicine. We select the treatment based on the biological markers. The mentioned drugs are being investigated as future treatments for depression.”
Q: “What new research, processes, etc., in your field make you most excited about the future, and why?”
Dr. Zarate: “I am truly excited about a number of promising insights on the horizon. One of them is that we are at the verge of having a new class of antidepressants, truly distinct in mechanism from existing antidepressants, for severe treatment-resistant depression, suicidal ideation, and anhedonia [inability to feel pleasure]. These symptoms can now be alleviated in hours instead of weeks. Next, we can work backward to try to decipher the mechanism of action of these new treatments that are radically distinct from existing treatments. This larger concept could then be applied to other severe mental disorders.”
Subscribe to our weekly newsletter to stay up-to-date on the latest breakthroughs in the NIH Intramural Research Program.
Related Blog Posts
This page was last updated on Wednesday, May 24, 2023
