Boosting Brain Activity to Suppress Snacking
Non-Invasive Stimulation Method May Improve Self-Regulation Around Food

New IRP research points to the possibility that a non-invasive brain stimulation technique could help people with obesity better control their food consumption.
Marketers make a living from the fact that merely seeing an advertisement for junk food can spur a sudden craving for potato chips or sugary cereal. Some people have an easier time than others resisting such urges, and over-consuming that sort of food can have problematic consequences for health. Findings from a recent IRP study suggest that stimulating a particular part of the brain might help people who struggle with obesity by enhancing their ability to control their desire to snack.1
While diets and exercise regimens can certainly help people with obesity lose weight and decrease their risk for health conditions like type 2 diabetes and heart disease, such lifestyle changes can be difficult to stick with. As a result, IRP senior investigator Marci Gluck, Ph.D., is investigating whether weight loss could be made easier by helping people increase their ‘inhibitory control,’ the ability to suppress an impulse to pursue a particular action. Numerous studies have established a link between inhibitory control and a part of the brain called the left dorsolateral prefrontal cortex (dlPFC), and still more research has suggested that consuming or seeing food activates neurons in that brain area less in people with obesity than in people with a lower weight.
“When people drive by McDonald’s, they might have trouble inhibiting their desire to stop there, for example,” says Dr. Gluck, the new study’s senior author. “There are probably some people who are affected more by these cues we see in our culture, possibly because they have less inhibitory control. Their brains are more driven to respond to those cues.”
“Maybe because there’s less activation in this brain area, it’s harder for some individuals to say no to those things,” adds IRP biostatistician Emma J. Stinson, who led the new study in Dr. Gluck’s lab.
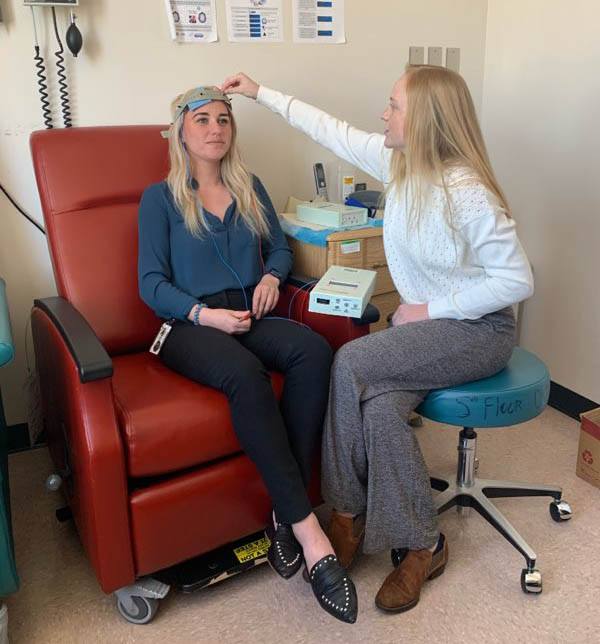
A member of Dr. Gluck’s research team practices setting up the transcranial direct current stimulation (tDCS) equipment on Emma Stinson (left), the new study’s first author.
In 2008, Dr. Gluck’s lab initiated a small clinical trial testing whether stimulating neurons in the left dlPFC with a non-invasive technique called transcranial direct current stimulation (tDCS) could help people with obesity regulate their food consumption and lose weight. Results from the trial published in 2017 showed that compared to study volunteers who received a placebo variety of fake, ‘sham’ stimulation, participants who received ‘active’ tDCS targeting the left dlPFC 15 times over the course of several weeks consumed less food during a ‘snack food taste test’ that provided them with unrestricted access to high-calorie snacks.2
In the new IRP study, Dr. Gluck’s team re-examined their data from that prior experiment to assess the relationship between dlPFC stimulation, food consumption during the snack food taste test, and performance on a behavioral task called the Go/No Go task. During that task, participants viewed pictures of low-calorie and high-calorie food items and were asked to press a button only when they saw a low-calorie food. Because the task involves resisting the desire to push the button in response to high-calorie foods, it is thought to be a useful way to measure inhibitory control.
The researchers found that the people who received tDCS to the left dlPFC improved significantly on the Go/No Go task over the course of the study, mistakenly pressing the button in response to high-calorie foods roughly half as often during their final assessment compared to their first try at the task. On the other hand, the participants who received the placebo sham stimulation did not noticeably improve on the task. When combined with the fact that participants who received tDCS also consumed less food during the subsequent snack food taste test than the placebo group, these results point to the possibility that the reduced food consumption was due to an improvement in inhibitory control among the people who received tDCS to the dlPFC.

Dr. Marci Gluck
What’s more, when looking solely at the participants who received the sham stimulation, those who did worse on the Go/No Go task tended to consume more food during the snack food taste test, lending credence to the idea that better inhibitory control can help people curb their food intake. However, when the researchers analyzed the data from everyone in the study, there was no statistically significant association between the amount of food participants consumed during the snack food taste test and the amount they improved on the Go/No Go task. As a result, while the findings are suggestive, they do not definitively prove that better inhibitory control was the reason the group who received tDCS decreased their snack consumption.
“I think if we’d had a few more people in the study, it might have shown that the tDCS was working through this inhibitory control mechanism to reduce snack food intake,” says Stinson.
“We don’t want to over-state our results, but I think we do have enough evidence to support doing another study on this,” adds Dr. Gluck.
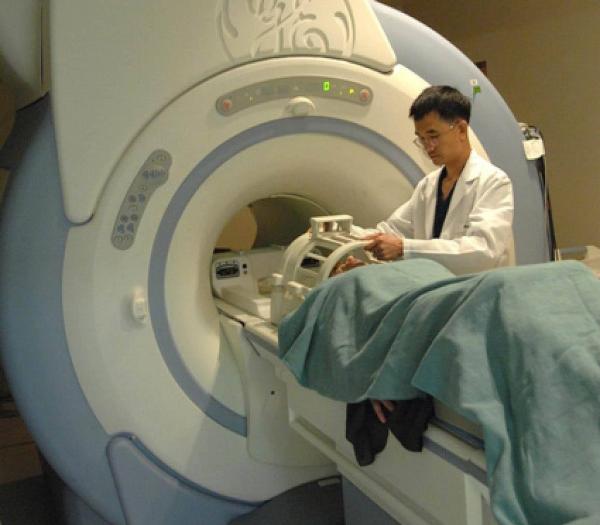
Follow-up studies by Dr. Gluck’s team will use a functional magnetic resonance imaging (fMRI) machine like this one to gauge how tDCS affects brain activity.
In fact, Dr. Gluck’s team has already begun a follow-up study that will use functional magnetic resonance imaging (fMRI) to see how stimulating the dlPFC with tDCS changes the way the brain responds to images of food in both the short and long term. If that study shows tDCS can enhance activity in the dlPFC and additional studies link that brain boost to decreased food intake or weight loss, then tDCS might eventually become another tool that doctors can use to help people with obesity lose weight.
“These new ways of stimulating brain activity are non-invasive, and I think that aspect of it is important,” Stinson says. “They can be used in conjunction with nutritional or behavioral interventions to create this package for a weight loss or weight maintenance plan.”
Subscribe to our weekly newsletter to stay up-to-date on the latest breakthroughs in the NIH Intramural Research Program.
References:
[1] Stinson EJ, Travis KT, Magerowski G, Alonso-Alonso M, Krakoff J, Gluck ME. Improved food Go/No-Go scores after transcranial direct current stimulation (tDCS) to prefrontal cortex in a randomized trial. Obesity. 2022 Oct;30(10):2005-2013. doi: 10.1002/oby.23529.
[2] Heinitz S, Reinhardt M, Piaggi P, Weise CM, Diaz E, Stinson EJ, Venti C, Votruba SB, Wasserman EM, Alonso-Alonso M, Krakoff J, Gluck ME. Neuromodulation directed at the prefrontal cortex of subjects with obesity reduces snack food intake and hunger in a randomized trial. Am J Clin Nurt. 2017 Dec;106(6):1347-1357. doi: 10.3945/ajcn.117.158089.
Related Blog Posts
This page was last updated on Wednesday, May 24, 2023
