Chemical Tag-Team Shows Promise as Diabetes Treatment
Therapeutic Strategy Enhances Natural Blood Sugar Control
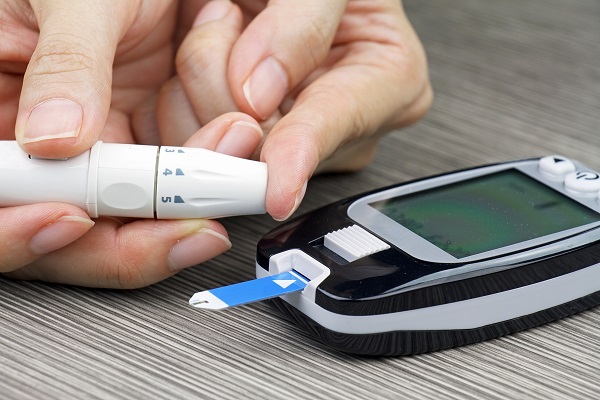
Patients with type 2 diabetes must carefully manage their blood sugar. New IRP research points to a potential therapeutic strategy that boosts the body’s natural ability to keep blood sugar in check.
Just like Sonny needed Cher to achieve music super-stardom and Stephen Curry needed Kevin Durant to win back-to-back NBA championships, sometimes a cell or molecule in the human body needs a partner’s assistance to work optimally. IRP researchers recently showed that a synergy between a lab-designed drug and a molecule naturally produced in the body could make for a promising therapy for type 2 diabetes.1
Diabetes occurs when blood sugar levels are chronically high, which damages many types of bodily tissues. The chemical insulin keeps blood sugar in check, but patients with type 2 diabetes require extra insulin to prevent dangerously high blood sugar because their cells don’t respond as strongly to it. While these individuals can control their illness with insulin injections, this self-managed treatment can require administering precise doses of insulin multiple times per day. Pharmacological interventions like the drug metformin can be easier to manage but have problematic side effects.
To make management of type 2 diabetes easier, researchers like IRP senior investigator Jurgen Wess, Ph.D., are pursuing treatments that boost the body’s ability to produce its own insulin. Many of these therapies affect the beta cells in the pancreas, which release insulin when a chemical called acetylcholine interacts with proteins on the beta cells called M3 receptors.
Scientists have discovered that molecules called ‘allosteric modulators’ interact with a different part of the M3 receptor than acetylcholine does and influence how much insulin a beta cell releases in response to acetylcholine. Just like the best basketball players make their teammates better, so-called ‘positive allosteric modulators,’ or PAMs, make acetylcholine a more potent stimulator of insulin secretion from beta cells.
“PAMs have the advantage that you maintain the physiological, temporal, and spatial mode of activation,” Dr. Wess explains. “The PAM only jumps into action when acetylcholine is released, and acetylcholine is only released in the pancreas when blood sugar increases. If you have a lot of acetylcholine, the PAM does a lot. If you have no acetylcholine, the PAM does nothing.”
For its recent study, Dr. Wess’s team tested a M3 receptor PAM discovered at Vanderbilt University2 on cells taken from a mouse beta cell tumor, which behave very similarly in many ways to normal beta cells but are easier to grow in the lab. Those cells secreted more insulin in response to a combination of acetylcholine and the PAM than acetylcholine alone. By itself, however, the PAM did not stimulate insulin release.
The scientists saw similar results in pancreatic islets, clusters of cells from the pancreas that contain beta cells along with cells that secrete other important chemicals. Pancreatic islets from both mice and humans released more insulin when exposed to acetylcholine and the PAM than when exposed to only acetylcholine.
In addition, giving the PAM to normal mice and obese mice with blood sugar problems caused the animals’ bodies to release more insulin when they were fed a sugar solution, resulting in a faster return to normal blood sugar levels. However, this effect did not occur in mice that lacked M3 receptors in their beta cells, confirming that the PAM exerts its therapeutic effects by interacting with those receptors.
“Not only were we able to see benefits in the normal mice, but we were also able to see that the compound’s effect was eliminated by just knocking out a single receptor subtype in a single cell type,” Dr. Wess says. “That made us really happy because that meant we had demonstrated the mechanism through which this compound exerts its effect. That made the story complete.”
Importantly, a dose of the PAM high enough to improve blood sugar control did not cause any side effects, although a higher dose did stimulate muscles in the mouse’s eyes that have the same M3 receptors as beta cells. Scientists will need to examine such potential side effects more closely before testing a PAM-based treatment strategy in clinical trials for type 2 diabetes. They will also need to develop more precisely targeted PAMs that only affect M3 receptors, since the PAM used in Dr. Wess’s study can also boost acetylcholine’s effect on two other types of acetylcholine receptor.
“Medicinal chemists need to come up with compounds that are truly selective M3 PAMs,” Dr. Wess says. “Using structure-guided drug design that looks at the structure of the space where the PAM binds to the M3 receptor, you may be able to modify the structure of this compound to prevent it from binding to other types of receptors.”
Subscribe to our weekly newsletter to stay up-to-date on the latest breakthroughs in the NIH Intramural Research Program.
References:
[1] Allosteric modulation of β-cell M3 muscarinic acetylcholine receptors greatly improves glucose homeostasis in lean and obese mice. Zhu L, Rossi M, Cohen A, Pham J, Zheng H, Dattaroy D, Mukaibo T, Melvin JE, Langel JL, Hattar S, Matschinsky FM, Appella DH, Doliba NM, Wess J. Proc Natl Acad Sci U S A. 2019 Aug 26. pii: 201904943. doi: 10.1073/pnas.1904943116. [Epub ahead of print]
[2] Chemical lead optimization of a pan G(q) mAChR M(1), M(3), M(5) positive allosteric modulator (PAM) lead. Part I: Development of the first highly selective M(5) PAM. Bridges TM, Kennedy JP, Cho HP, Breininger ML, Gentry PR, Hopkins CR, Conn PJ, Lindsley CW. Bioorg Med Chem Lett. 2010 Jan 15;20(2):558-62. doi: 10.1016/j.bmcl.2009.11.089.
Related Blog Posts
This page was last updated on Tuesday, May 23, 2023
