Star-Shaped Brain Cells May Contribute to Marijuana Addiction
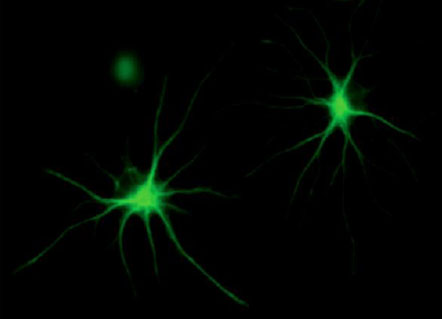
IRP researchers have found evidence that star-shaped brain cells called astrocytes, pictured above, may play a role in the brain systems that cause people to get hooked on marijuana.
The recent spate of state laws legalizing marijuana for medical or recreational purposes has prompted concerns that increased marijuana use will boost the number of people who become dependent on and abuse the drug, a condition known as cannabis use disorder (CUD). Treating the growing number of patients with CUD will require a greater understanding of how chronic marijuana use can lead to addiction. New IRP research has revealed that star-shaped brain cells called astrocytes may play a role in the pleasurable effects of marijuana and contribute to the drug’s addictive properties.1
Marijuana is the most commonly used illegal substance in the U.S., and estimates suggest that nearly 10 percent of users develop CUD at some point in their lives.2 THC, a member of a molecular family called cannabinoids and the primary cause of marijuana’s psychological effects, has long been known to increase the release of the chemical dopamine in brain areas involved in reward and addiction. More recent studies have also found evidence that THC can affect the release of another chemical, called glutamate, in these and other areas of the brain. Since glutamate can spur neurons to spit out dopamine, scientists have long wondered about its role in the development of marijuana dependence.
More than a decade ago, researchers discovered that giving rats a compound that blocked chemical docking stations in the brain called alpha-7 nicotinic receptors eliminated some of THC’s abuse-related behavioral and neurochemical effects.3 These receptors are found on the surface of certain neurons and on astrocytes, brain cells that play a supportive role in many neurological processes and can produce glutamate. Unfortunately, using such compounds to block alpha-7 receptors was a less-than-ideal approach for prospective CUD therapies.
“These drugs would have a lot of side effects, so they have limited clinical utility,” says IRP staff scientist Zuzana Justinova, M.D., Ph.D., the new study’s lead author. “We were wracking our brains at the time to figure out how we can target alpha-7 receptors in a potentially safer way, and we found KYNA.”
KYNA, short for kynurenic acid, is produced by astrocytes and inhibits alpha-7 receptors in the brain in a manner different from molecules that block the receptors. Promisingly, in a 2013 study, Dr. Justinova and her colleagues found that a drug called Ro 61-8048 that significantly increased KYNA levels and decreased dopamine release in reward-related brain areas in rats. The Ro compound also curbed abuse-related behaviors in monkeys given THC and rats given synthetic cannabinoids.4 This suggested that KYNA’s inhibitory effect on alpha-7 receptors prevented THC from triggering the dopamine release thought to contribute to addiction.
In the new study, Dr. Justinova and her collaborators from the IRP, University of Maryland, University of Cagliari, and University of Ferrara showed for the first time that THC increases glutamate levels and decreases KYNA levels in three reward-related areas of rats’ brains, bolstering the idea that glutamate, like dopamine, may be involved in marijuana’s psychological effects. THC also increased electrical firing between neurons in those brain regions, but when the animals were given both THC and the KYNA-boosting Ro drug, THC no longer increased glutamate levels or neuronal activity in those areas.
Since KYNA affects alpha-7 receptors on both neurons and astrocytes, these findings led the team to hypothesize that THC might spur both types of cells to release glutamate. Further experiments using isolated rat astrocytes in petri dishes confirmed this idea: both THC and a synthetic cannabinoid spurred the astrocytes to produce glutamate, but not when KYNA was also added to the petri dishes.
“We were surprised by how well the experiments with the astrocytes worked,” Dr. Justinova says. “They really nicely mirrored what we saw in the live animal studies.”
The new study’s results suggest that THC stimulates both neurons and astrocytes to release glutamate and that this process can be inhibited by increased KYNA release from astrocytes. If these ideas hold up to further scrutiny, it may be possible to curb the addictive properties of marijuana, and possibly other drugs like nicotine, by encouraging astrocytes to release more KYNA, as this might short-circuit the drugs’ effects on glutamate and dopamine release in reward-related brain areas.
“Understanding the relationship between THC, glutamate, and KYNA could lead to new therapeutic approaches for the treatment of cannabis use disorder,” Dr. Justinova says. “It could also provide new insights into the mechanisms that underlie the therapeutic and also the abuse-related effects of cannabinoids like THC, so I think it’s an interesting avenue to pursue in the future.”
Subscribe to our weekly newsletter to stay up-to-date on the latest breakthroughs in the NIH Intramural Research Program.
References:
[1] Astrocytic Mechanisms Involving Kynurenic Acid Control Δ9-Tetrahydrocannabinol-Induced Increases in Glutamate Release in Brain Reward-Processing Areas. Secci ME, Mascia P, Sagheddu C, Beggiato S, Melis M, Borelli AC, Tomasini MC, Panlilio LV, Schindler CW, Tanda G, Ferré S, Bradberry CW, Ferraro L, Pistis M, Goldberg SR, Schwarcz R, Justinova Z. Mol Neurobiol. 2018 Aug 27. doi: 10.1007/s12035-018-1319-y.
[2] Cannabis use disorders in the USA: prevalence, correlates and co-morbidity. Stinson FS1, Ruan WJ, Pickering R, Grant BF. Psychol Med. 2006 Oct;36(10):1447-60. Epub 2006 Jul 20.
[3] Nicotinic alpha 7 receptors as a new target for treatment of cannabis abuse. Solinas M, Scherma M, Fattore L, Stroik J, Wertheim C, Tanda G, Fratta W, Goldberg SR. J Neurosci. 2007 May 23;27(21):5615-20.
[4] Reducing cannabinoid abuse and preventing relapse by enhancing endogenous brain levels of kynurenic acid. Justinova Z, Mascia P, Wu HQ, Secci ME, Redhi GH, Panlilio LV, Scherma M, Barnes C, Parashos A, Zara T, Fratta W, Solinas M, Pistis M, Bergman J, Kangas BD, Ferré S, Tanda G, Schwarcz R, Goldberg SR. Nat Neurosci. 2013 Nov;16(11):1652-61. doi: 10.1038/nn.3540. Epub 2013 Oct 13.
Related Blog Posts
This page was last updated on Tuesday, January 30, 2024
