Postdoc Profile: COVID-19 Provides New Opportunities for Virus Science
Dr. Alberto D. López-Muñoz Pivots to New Research Focus Amidst Pandemic

IRP postdoctoral fellow Alberto D. López-Muñoz
Like all virologists, IRP postdoctoral fellow Alberto D. López-Muñoz, Ph.D., knew a global pandemic was sadly inevitable. No one could predict exactly when, but it was just a matter of time until a novel virus would make its way around the globe. Nevertheless, when the COVID-19 pandemic hit, caused by a virus called SARS-CoV-2, even Dr. López-Muñoz was surprised by how rapidly his career transformed as he switched gears study the novel contagion.
Dr. López-Muñoz arrived at the National Institute of Allergy and Infectious Diseases (NIAID) in September 2019 with the intention of spending his postdoc studying the influenza virus responsible for the seasonal flu. After the COVID-19 pandemic began a few months later, he began studying the novel coronavirus, taking advantage of his expertise on the herpes simplex virus that had been the focus of his Ph.D. research in Madrid, Spain.
“Although coronaviruses were not my major area of expertise, immune modulation strategies are similar between viruses, so I thought I could apply some of the same tools and techniques that I learned with herpes to SARS-CoV-2,” he explains.
The various proteins a virus can create are encoded in its genome. Compared to the herpes virus, SARS-CoV-2 has a much smaller genome, which means it produces fewer proteins that it can use to try and fool the human immune system. Over the last year, Dr. López-Muñoz and his colleagues investigated many SARS-CoV-2 proteins to see which ones interacted with the human immune system.
Dr. López-Muñoz and his colleagues ultimately identified one particularly interesting viral protein that inhibits the function of cytokines. Cytokines are critical for orchestrating a healthy immune response and their inhibition leads to a dampened reaction. What’s more, this particular viral protein appeared not only in infected cells, but also in nearby uninfected cells.
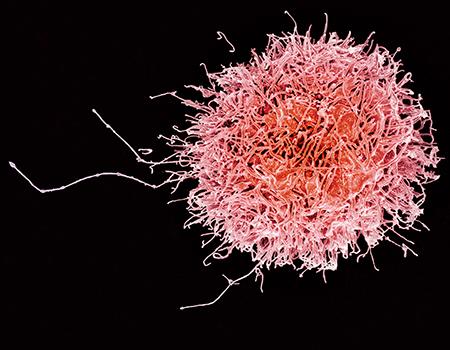
Overreactions by immune cells like this one are thought to be responsible for the life-threatening cytokine storms that occur in some COVID-19 patients.
Dr. López-Muñoz speculates that this may mean these uninfected cells are unable to trigger a healthy cytokine response and therefore may be more susceptible to infection. This may explain how COVID-19 can spread throughout the human body while evading detection at first, causing the body to be overwhelmed by it later. The body then overcompensates in its response, producing a potentially life-threatening immune overreaction called a cytokine storm.
“These hidden roles of SARS-CoV-2 proteins in immune modulation could help to explain the mechanisms behind the most severe symptoms associated with COVID-19,” says Dr. López-Muñoz.
As the U.S. endures a fourth wave of the COVID-19 pandemic, Dr. López-Muñoz continues to investigate the hidden roles of SARS-CoV-2 proteins. He hopes that his work will shed light on some of the particularly dangerous aspects of COVID-19 infections and ultimately increase our understanding of how to prevent them. In a hopeful turn of events, the SARS-CoV-2 protein Dr. López-Muñoz and his colleagues identified may be the key to accomplishing that goal. They have found that human antibodies can bind to this viral protein and direct the immune system to attack and destroy it, which may mean this protein could be used in treatments and vaccines for COVID-19.
Dr. López-Muñoz credits his supportive mentor, IRP senior investigator Jonathan Yewdell, M.D., Ph.D., for his ability to rapidly switch his focus to SARS-CoV-2. However, Dr. López-Muñoz also acknowledges that he was in the right place at the right time to study the new virus. If he had arrived at NIH sooner, he would likely have been too far into a different research project to switch gears when the pandemic hit. The funding and resources he had access to at NIAID also helped him make the pivot to studying COVID-19.
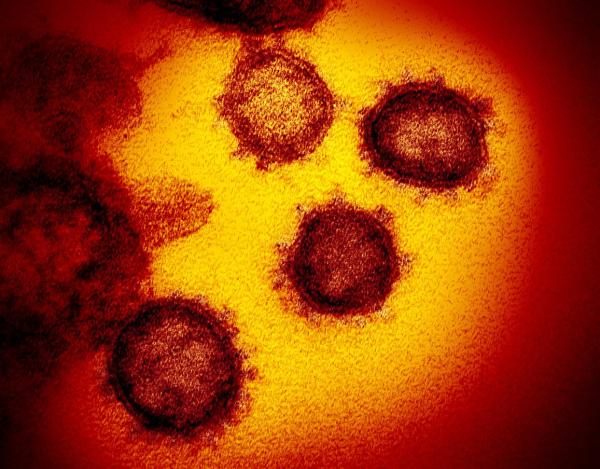
This transmission electron microscope image shows SARS-CoV-2, the virus that causes COVID-19, isolated from a patient in the U.S., emerging from the surface of cells cultured in the lab.
Yet another perk of working as a postdoc at NIAID was the chance to witness first-hand the development of the NIAID-Moderna COVID-19 vaccine. Dr. López-Muñoz even volunteered for the Phase III clinical trial testing the vaccine and received his first shot in August 2020.
“I was able to witness how the whole process was orchestrated from the beginning, and for me it was very inspiring,” he explains. “I wanted to contribute.”
Now, more than a year later, he reflects on that first immunization as the moment “which made me feel it was going to be okay.” However, like so many others, Dr. López-Muñoz has experienced his share of dark moments during the pandemic. As a visiting scientist from Europe, he was restricted from travelling to see his family members for many months. These restrictions were particularly frustrating because he was vaccinated for much of that period.
Despite these challenges, Dr. López-Muñoz chooses to focus on the positive: the opportunity to study SARS-CoV-2 and further his research career as a molecular virologist at one of the world’s pre-eminent institutions for biomedical research.
“I have kept in mind that this is a unique opportunity to do the best science I can do,” he says. “That has kept me in a positive attitude.”
Subscribe to our weekly newsletter to stay up-to-date on the latest breakthroughs in the NIH Intramural Research Program.
Related Blog Posts
This page was last updated on Monday, January 29, 2024
