IRP’s Anthony Fauci Talks COVID-19 With Stephen Curry
Infectious Disease Expert Interviewed by NBA Superstar
As the COVID-19 illness has continued to spread, so has anxiety, fear, and uncertainty. Now more than ever, we need communicators who can provide clear explanations about the latest research and public health guidelines.
IRP senior investigator Anthony Fauci, Ph.D., has been one of the most prominent voices providing information about the novel coronavirus over the past several weeks. Dr. Fauci, who serves as director of the NIH’s National Institute of Allergy and Infectious Diseases (NIAID), seems to be doing everything he can to make sure the American public has the best information available about the current situation, from speaking at White House press briefings to appearing on television shows like The Daily Show with Trevor Noah. Last Thursday, March 26, Dr. Fauci participated in a live Q&A with NBA superstar Stephen Curry on Curry’s Instagram page. Read on for a few highlights from their discussion, or click on the video below to watch the entire conversation.
Basketball superstar Stephen Curry (left) chatted with the IRP’s Anthony Fauci (right) about COVID-19 on Instagram Live on March 26.
On the differences between the novel coronavirus and the seasonal flu
“It’s very, very much more transmissible than flu, and more importantly, it’s significantly more serious…The overall mortality of seasonal flu that you and I confront every year is about 0.1 percent. The overall mortality of coronavirus is about 1 percent, and sometimes — like in China — it was up to 2 or 3 percent, which means it’s 10 times more serious than the typical influenza. So when people kind of compare it, in some respects it has some similarities, but it’s really, really different in its degree of seriousness.”
On whether contracting the novel coronavirus confers immunity to future infections by the same illness
“We haven’t done the specific testing to determine that, but if this acts like every virus similar to it that we know, the chances are overwhelming that if you get infected [and] recover from infection, that you are not going to get reinfected with the same virus, which means you can then safely go out into the community and feel immune so that you can not only protect yourself, get back to work, get back to your job, but you’ll also be able to have what you refer to as ‘herd immunity.’ [When] enough people [have] recovered in a community, that gives the virus very little chance to spread rapidly.”
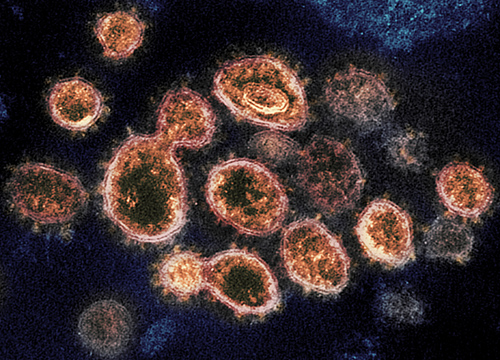
This transmission electron microscope image shows SARS-CoV-2, the virus that causes COVID-19, isolated from a patient in the U.S.
On how the changing seasons could affect the transmission of COVID-19
“Viruses tend to do poorly in warm, moist weather and do quite well in cold, dry weather, and that’s one of the reasons why — in addition to the fact that in the warm weather you’re more outside and not confined in a room — that these kinds of respiratory viruses tend to go down as you get to the summer months…We don’t know whether this is going to happen with this virus because this is the first time we’ve ever dealt with this virus, so it’s not an unreasonable assumption to think that it’s going to go down, but you don’t want to count on it.”
On our ability to more effectively contain the virus if it re-emerges in the fall after a summer hiatus
“I think and I hope — and it’s not just hope because I think, if we do it right, it will happen this way — that we will get enough experience so that, when it does come back, we will be able to immediately identify, isolate, and contact-trace. And if you do that effectively, you don’t have an outbreak. You contain it at a very low level, which would mean we won’t have to lock down again…It will be much different than what we’re doing right now.”
On how long it will take to develop a COVID-19 vaccine
“We have started on the development of a vaccine faster than ever in the history of any virus, from the time [the virus] was discovered to the time that we made [the vaccine] and put it into a trial. But when you test a vaccine, it’s multiple phases. The first thing you’ve got to do is make sure it’s safe. We started that a couple weeks ago. When you find out it’s safe and that it induces the kind of response you want it to, then you do it in a lot of people. The first stage you have to be careful — it’s like 45 people. Then you go into hundreds, if not thousands, of people in what’s called a phase 2/3 trial to determine if it works…If we really push, we hope that we will know by the time we get into next winter whether or not we have something that works.”
On the biggest misconception about COVID-19 that Dr. Fauci has encountered
“This dichotomy between people who are being frightened to death of [COVID-19] versus people who don’t even believe it and think it’s something trivial that you don’t have to worry about. I’d like to get the people in the country to realize that we are dealing with a serious problem…We’ve modified our lives. It’s not convenient to lock yourself in…but we’re going through a period of time now where we’ve got to — as a country — pull together, don’t get frightened, don’t get intimidated, use the energy to be able to confront it and do the kinds of things that will put an end to it. I want to get rid of that misconception that there’s extremes: either the world is going to end, or we don’t want to do anything. It isn’t that. It’s somewhere in the middle.”
Subscribe to our weekly newsletter to stay up-to-date on the latest breakthroughs in the NIH Intramural Research Program.
Related Blog Posts
This page was last updated on Monday, January 29, 2024
