Non-Toxic Drug Could Increase Availability of Organ Transplants
Treatment Regimen Allows Genetically Mismatched Skin Grafts in Mice
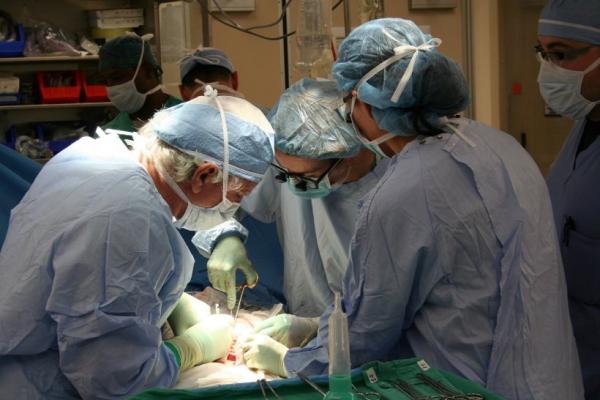
New IRP research examined a therapeutic approach that could dramatically reduce the risks of organ transplantation, potentially allowing many more patients to undergo the life-saving procedure.
Thousands of patients who need an organ transplant die each year before a donor can be found. A new IRP study has identified a safer way to prevent a transplant recipient’s body from attacking a genetically dissimilar donor organ, which could dramatically expand the pool of potential organ donors.1
Finding organs for the 100,000 Americans currently on the national organ transplant waiting list is difficult not only because of the limited supply of donors but also because the donor and recipient must have an identical – or at least highly similar – set of genes called the major histocompatibility complex (MHC). Unfortunately, most patients cannot find an MHC-matched donor. The larger this genetic mismatch, the more likely the recipient’s body will attack the new organ, a potentially life-threatening complication called rejection that can occur even with a perfect MHC match.
Doctors try to prevent rejection with ‘immunosuppressive’ drugs that stifle recipients’ immune systems, but this leaves them vulnerable to infections. Moreover, many patients must take these drugs for the rest of their lives.
“Sometimes transplantation just replaces one disease for another — all these terrible things can happen,” says IRP senior investigator Philip Murphy, M.D., the new study’s senior author.
Scientists have found they can prevent rejection after MHC-mismatched organ transplants without using immunosuppressive drugs by first transplanting bone marrow from the organ donor to the recipient. The new bone marrow contains cells called stem cells that manufacture blood cells genetically identical to the bone marrow donor’s. This creates an immune system in the recipient comprised of a mix of the donor’s and recipient’s cells, and this hybrid immune system will not attack a transplanted organ that comes from the bone marrow donor.
For a bone marrow transplant to be successful, however, clinicians have to destroy enough of the recipient’s own blood-producing stem cells that the donated cells have room to take root, a process called ‘conditioning.’ Current conditioning methods, such as radiation and chemotherapy, can cause severe side effects because they wantonly destroy many types of cells.
In the new study, the IRP scientists used a drug developed by collaborators at Harvard University that selectively destroys blood-producing stem cells. The researchers treated mice with the compound, called CD117-ADC, and then gave them bone marrow transplants from mice with completely different MHC genes, followed by a 30-day course of immunosuppressive drugs. Without the CD117 treatment, the transplanted bone marrow produced very few new blood cells in the recipient mice. The treated mice, on the other hand, had many more blood cells that were identical to those of the donor mice, and in almost all of the treated mice those levels remained high for the entire duration of the experiment — nearly two years — without the need for more immunosuppressive drugs.
The researchers then transplanted skin from the bone marrow donor mice and a third set of unrelated mice onto the mice that had received the bone marrow transplants. The bodies of untreated recipient mice attacked both skin grafts, while the animals given CD117-ADC before the bone marrow transplant only rejected the skin grafts from the unrelated mice. This suggests that their bodies accepted the skin from the bone marrow donor as if it were their own but still retained the ability to attack other foreign cells, like the skin from the unrelated mice that had not donated bone marrow. And all this occurred without any significant side effects from the treatment.
“My hope is that this can be developed into a method of enabling universal transplantation in humans and be applicable to any disease that requires a donor cell, tissue, or organ,” Dr. Murphy says. “If we succeed, anybody could potentially be a donor for anybody else, largely resolving the donor shortage. It would also make transplant safer because all the toxicities that occur from the immunosuppression and the conditioning that people use now would be a thing of the past.”
The team’s approach could also boost the effectiveness of MHC-mismatched bone marrow transplants, which are sometimes used to cure genetic conditions that cause defects in blood cells. But before a clinical trial can test CD117-ADC in human transplant recipients, the IRP researchers need to conduct further experiments to refine the treatment strategy and test its effects on other types of transplants and in larger animal models.
“These are early days and there’s going to be a lot of heavy lifting,” he says, “but this method is so targeted and it’s such a simple idea that we’re cautiously optimistic it can go the distance to the clinic.”
Subscribe to our weekly newsletter to stay up-to-date on the latest breakthroughs in the NIH Intramural Research Program.
References:
[1] Hematopoietic chimerism and donor-specific skin allograft tolerance after non-genotoxic CD117 antibody-drug-conjugate conditioning in MHC-mismatched allotransplantation. Li Z, Czechowicz A, Scheck A, Rossi DJ, Murphy PM. Nat Commun. 2019 Feb 6;10(1):616. doi: 10.1038/s41467-018-08202-w.
Related Blog Posts
This page was last updated on Tuesday, January 30, 2024
