Study Explores Sex Differences in Flu
Differences in Flu-Fighting Antibodies Could Explain Women’s Greater Susceptibility

New IRP research points to a possible biological reason why the flu tends to be more serious in women than men.
It is well-known that COVID-19 infections are more often life-threatening in the elderly and individuals with chronic medical conditions like obesity, but the novel coronavirus isn’t the only infectious disease that more severely affects certain groups of people. A new IRP study explored a possible biological reason why women tend to experience worse flu infections and suggests a way to potentially improve the effectiveness of flu vaccines for everyone.1
Whenever a large flu outbreak occurs, like the 1918 Spanish flu pandemic or the global spread of ‘swine flu’ in 2009, scientists sift through the data to see how people of different ages, ethnicities, and genders were affected. Many of these studies have shown that the flu affects women more strongly than men. What’s more, the immune responses of men and women to flu vaccines can also differ wildly, with one study showing that a half-dose of a flu vaccine caused women to produce just as many flu-fighting antibodies as men did when given a full dose of the same vaccine.2
“We don’t understand a lot of things about the course of these respiratory virus infections,” says Luca Giurgea, M.D., an IRP clinical fellow who studies the flu in the lab of IRP senior investigator Matthew Memoli, M.D., M.S. “When some people do fine and some get really sick, it’s not clear what’s different about those people, let alone what makes someone not get sick at all. We don’t understand all the factors that are at play, and I think this male-female dichotomy is a very high-yield thing to go after to explore what’s really driving these differences that have very real ramifications for disease management.”

More From the IRP
Blog
Mold Exposure Sets Stage for Severe Flu
However, ‘retrospective’ studies that look back at past outbreaks to learn about the flu’s differing effects in men and women are complicated by many non-biological factors. For example, in many cultures, women tend to spend more time with children than men do, resulting in greater exposure to the respiratory viruses that are common among children. Researchers attempt to overcome these issues with ‘human challenge studies,’ in which participants are exposed to identical doses of a virus and their experiences are examined in a standardized manner.
The new IRP study, led by Dr. Giurgea and Dr. Memoli, combined data from four human challenge studies that Dr. Memoli’s lab had previously conducted. Consistent with prior research, they found that the men in the studies experienced slightly fewer flu symptoms on average compared to the women after they were exposed to the virus. Men were also 16 percent less likely than women to have any symptoms at all.
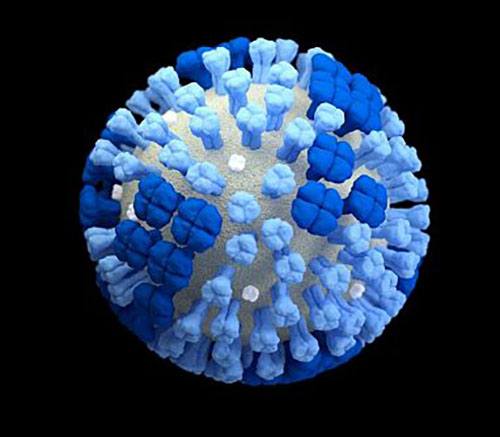
Image credit: CDC/Dan Higgins
Illustration of a whole influenza virus with a light grey surface membrane and the virus’ surface proteins hemagluttinin (light blue) and neuraminidase (dark blue).
The researchers also examined the levels of two flu-fighting antibodies in the participants’ blood before and after exposure to the virus. One of these antibodies inhibits a flu protein, called hemagglutinin, that the virus uses to gain entry into cells. The other inhibits a flu protein called neuraminidase, which helps the virus extract itself from a cell it has infected so it can proceed to infect another cell.
“When you hear the names of different flu strains, like H1N1 or H3N2, that refers to the type of hemagglutinin — the H — and the type of neuraminidase — the N — that it has,” Dr. Giurgea explains.
Unsurprisingly, levels of antibodies against hemagglutinin and neuraminidase increased after flu exposure in both men and women. However, whereas levels of antibodies against hemagglutinin were similar in men and women four and eight weeks after exposure, men had much higher levels of antibodies against neuraminidase at those time points. Moreover, the more neuraminidase antibodies a person had at baseline prior to flu exposure, the less severe his or her illness was afterwards, including having fewer symptoms, having symptoms for a shorter period of time, being more likely to be completely asymptomatic, and being less likely to have detectable levels of the virus in the nose. Pre-exposure levels of neuraminidase antibodies were lower on average in women than men, but the difference did not quite reach statistical significance.
Standardizing, and maybe increasing, the amount of flu neuraminidase protein in vaccines could potentially boost their effectiveness.
Overall, the new study suggests that differences in the levels of neuraminidase-inhibiting antibodies may partly explain why women tend to experience worse flu infections than men. The results also bolster the argument, long championed by Dr. Memoli’s lab, that scientists and vaccine developers should pay more attention to the importance of antibodies against neuraminidase. Right now, flu vaccines contain a standard amount of the flu hemagglutinin protein, but the amount of neuraminidase in them can vary widely. Addressing this imbalance could make seasonal flu vaccines better at preventing illness.
“Flu vaccines have had underwhelming effectiveness sometimes,” Dr. Giurgea says. “The flu is a rapidly mutating virus, and I think adding the neuraminidase could particularly help against the mutation problem because we’d be hitting two targets — now the virus would have to mutate both its hemagglutinin and neuraminidase in order to evade the vaccine. I think creating vaccines that elicit this multi-faceted immune response against multiple targets might help alleviate those types of problems.”
Subscribe to our weekly newsletter to stay up-to-date on the latest breakthroughs in the NIH Intramural Research Program.
References:
[1] Sex Differences in Influenza: The Challenge Study Experience. Giurgea LT, Cervantes-Medina A, Walters K, Scherler K, Han A, Czaikowski LM, Baus HA, Hunsberger S, Klein SL, Kash JC, Taubenberger JK, Memoli MJ. J Infect Dis. 2021 Aug 23;jiab422. doi: 10.1093/infdis/jiab422.
[2] Half- vs full-dose trivalent inactivated influenza vaccine (2004-2005): age, dose, and sex effects on immune responses. Engler RJM, Nelson MR, Klote MM, VanRaden MJ, Huang C, Cox NJ, Klimov A, Keitel WA, Nichol KL, Carr WW, Treanor JJ, Walter Reed Health Care System Influenza Vaccine Consortium. Arch Intern Med. 2008 Dec 8; 168(22):2405-14. doi: 10.1001/archinternmed.2008.513.
Related Blog Posts
This page was last updated on Tuesday, May 23, 2023
