Experimental Psoriasis Drug Comes With An ‘On-Off’ Switch
IRP Research Could Lead to Light-Activated Treatments for Numerous Diseases

IRP researchers recently created an experimental treatment for psoriasis that can be switched on with violet light and switched off with green light.
Many helpful contraptions we use every day would be problematic if we couldn’t turn them off when we didn't need them. After all, you wouldn’t want to leave your oven on when you’re out of town, and most people wouldn’t sleep well with their bedside lamp on all night. Many medical treatments would benefit from the same flexibility, but creating such treatments is no easy task. IRP researchers recently took a significant step forward in this area by creating an experimental treatment for an irritating skin condition that can be activated and inactivated using different colors of light.1
As annoying as poison ivy or a mosquito bite might be, they aren’t a constant nuisance for most of us. Unfortunately, people with psoriasis constantly deal with itchy, inflamed, and sometimes painful patches of skin that can be so uncomfortable that they interfere with sleep or everyday tasks. While there are treatments for the ailment, there is no cure, and current therapies can have significant side effects.
IRP senior investigator Kenneth Jacobson, Ph.D., ended up in the field of psoriasis drug development largely by accident. Years ago, he became interested in figuring out how to stimulate receptors on the surface of cells for a chemical called adenosine that the body naturally produces. We now know activating these adenosine receptors has an anti-inflammatory effect that can help curb psoriasis symptoms, but his IRP team started its experiments with a particular subtype of adenosine receptor, known as A3, even before we knew its therapeutic applications.
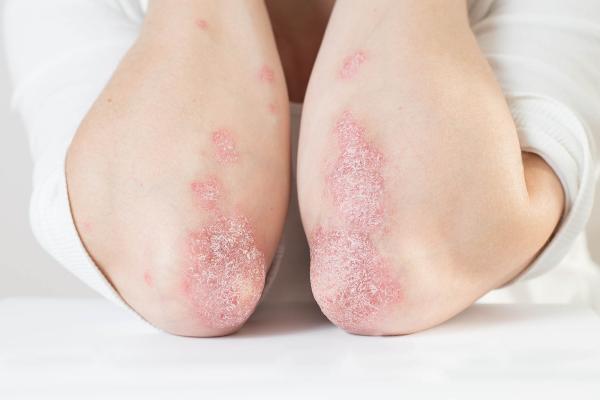
Psoriasis causes inflamed, itchy, and sometimes painful rashes like these.
“We jumped into the challenge of making chemicals that activate A3 receptors as soon as the receptor was cloned, before anyone had any idea what it was good for,” says Dr. Jacobson, the senior author of the new IRP study. “That’s what we can do in the NIH Intramural Research Program: we can go on a hunch and be more exploratory and do what would otherwise be considered more ‘high-risk’ science.”
That exploratory work would eventually allow Dr. Jacobson’s team to create a drug that alleviates psoriasis by activating the A3 receptor, which is now being tested in clinical trials by pharmaceutical company Can-Fite Biopharma and has shown similar effectiveness to existing therapies, but with much fewer side effects. In the new study, Dr. Jacobson and his collaborators took advantage of discoveries made over the past two decades about the A3 receptor to tweak a part of that psoriasis drug so they could switch the treatment on and off.
“When we first made the drug, we didn’t have a good idea of the shape of the A3 receptor, so our research wasn’t informed by the three-dimensional fit of the drug into it,” Dr. Jacobson recalls. “Now we know what’s important for that fit. Part of the drug molecule is kind of sticking up, and it’s in a region that has some flexibility — it can move around a little. We reasoned that instead of a chemical group that would stick straight up, putting a group there that would kind of fold upon itself when you shine one wavelength of light on it and open up when you shine another wavelength on it would allow us to switch it from inactive — because it wouldn’t have enough room to fit well into the receptor when it’s folded — to active — because when that part is opened up and extended, it would have enough room to fit.”
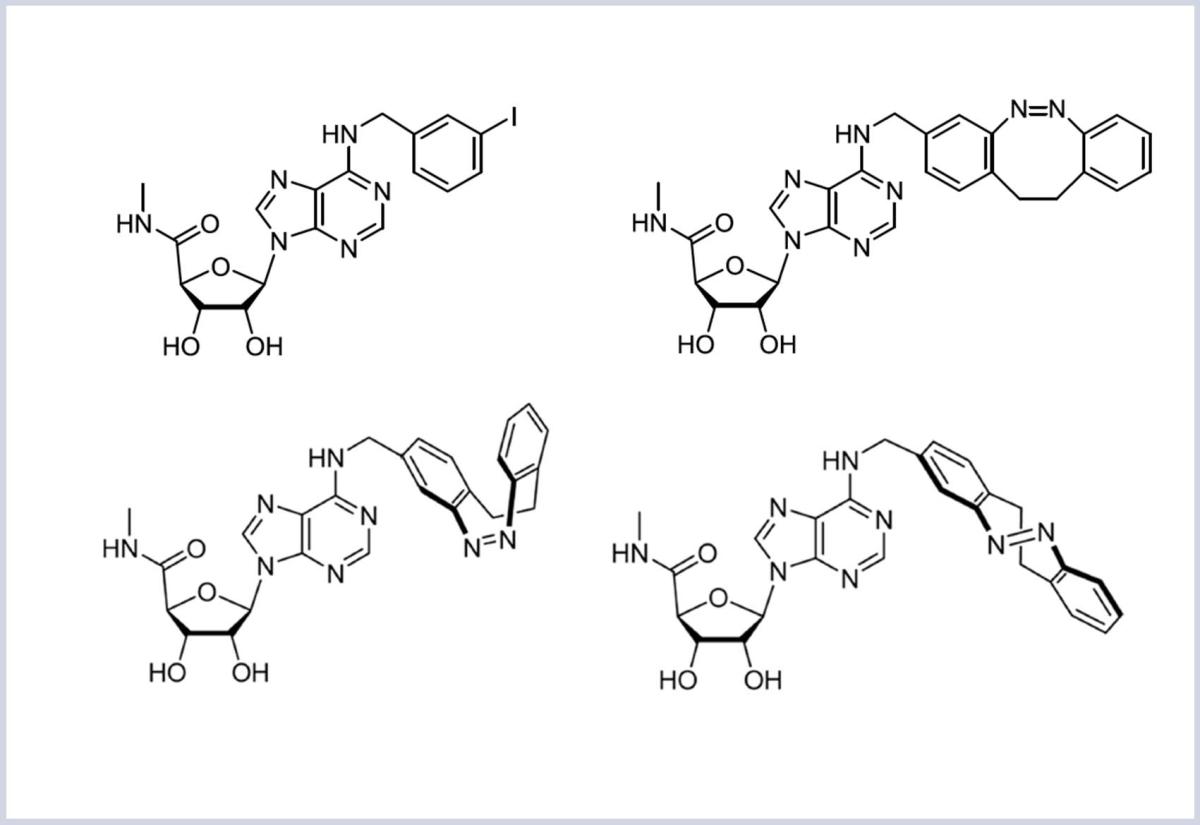
The image in the top-left corner shows the molecular structure of the original psoriasis drug, while the image to its right shows the structure of the light-activated version. Green light causes the modified part of the drug molecule to fold in on itself (bottom-left), making it inactive, while violet light causes that part of the molecule to extend (bottom-right), thereby activating the drug.
Even better, while some molecular components make a drug permanently active after exposure to the right type of light, the particular molecular group Dr. Jacobson’s team used doesn’t have this problem. Their experiments showed the modified molecule switches into the active state in response to violet light and back into the inactive state when exposed to green light, and it can do this over and over again. Moreover, just like the original, unmodified drug, the light-activated version stimulates the A3 receptor strongly at a reasonable dose but doesn’t have much of an effect on other types of adenosine receptors, which is the reason the original drug has so few side effects.
Of course, the next step was to see if the modified drug could still treat symptoms of psoriasis, so the researchers injected a molecule called IL-23 into the ears of mice in order to trigger inflammation similar to what occurs in psoriasis. Shining light on the inflamed ear did not have any therapeutic effect on untreated mice, and neither did the modified drug when it was given to the mice in its inactive state. However, shining the right wavelength of light on the mouse’s ear in the days after administering the treatment led to a reduction in inflammation. On the other hand, this did not occur when the mice were also given a drug that blocks A3 receptors, proving that the therapeutic effect depended on activation of those receptors by the light-sensitive drug.
“A lot of groups have studied light-activated drugs, and it’s an idea that has been around for a long time, but even so, there is no FDA-approved drug that uses this kind of shape-changing group,” Dr. Jacobson says.

Dr. Kenneth Jacobson
Dr. Jacobson emphasizes that the light-activated drug used in the new study is not likely to end up as an approved medical treatment, but that wasn’t his goal in the first place. Instead, he hopes that the study provides proof-of-principle for others who want to use a similar strategy to create light-sensitive drugs, whether for psoriasis or for other conditions. Indeed, since the A3 receptor is just one member of a broad class of so-called ‘G protein-coupled receptors,’ the study’s approach could have applications for treating a wide range of illnesses — although more work will be required to figure out the best way to activate light-sensitive drugs designed to target internal organs rather than the skin.
“There are many drugs that work through this family of receptors, so we wanted to come up with a clear way to switch the activity of a drug that affects these receptors using light,” Dr. Jacobson says. “I think there’s a future for this compound as a research tool and for applying this same principle for other compounds that target these sorts of receptors.”
Subscribe to our weekly newsletter to stay up-to-date on the latest breakthroughs in the NIH Intramural Research Program.
References:
[1] López-Cano M, Scortichini M, Tosh DK, Salmaso V, Ko T, Salort G, Filgaira I, Soler C, Trauner D, Hernando J, Jacobson KA, Ciruela F. Photoswitchable Diazocine Derivative for Adenosine A3 Receptor Activation in Psoriasis. J Am Chem Soc. 2025 Jan 8;147(1):874-879. doi: 10.1021/jacs.4c13558.
Related Blog Posts
This page was last updated on Tuesday, April 1, 2025
