Postdoc Profile: Finding the Narrative Behind the Numbers
Dr. Shameka Poetry Thomas Documents Black Women’s Experiences With Race and Racism

IRP postdoctoral fellow Shameka Poetry Thomas
The numbers are clear: Black women are three to four times more likely to die from pregnancy-related causes than White women in the United States. However, the reasons why are less clear. By listening to patient’s stories, IRP postdoctoral fellow Shameka Thomas, Ph.D., hopes to pinpoint potential explanations for this racial health disparity.
“We are losing mothers and children because we are simply not listening,” Dr. Thomas says.
Trained as a medical sociologist at the University of Miami, Dr. Thomas has devoted her career to documenting the lived experiences of patients of color, particularly women, who are perceived as Black.1 Dr. Thomas contextualizes patient’s narratives within a framework of ‘street race,’ which refers to how a person’s racial identity is perceived by others, regardless of their self-reported racial identity. Examining the influence of street race on women’s healthcare experiences, she explains, allows researchers to determine how health disparities are influenced by “how others see you.”
Patients have shared with her countless personal examples of how racial bias has reduced their access to healthcare. For example, women have told her that healthcare providers often assume they lack appropriate insurance or are seeking drugs, and these assumptions lead to delays receiving care. Many patients also describe various strategies they have used to attempt to reduce biased treatment, such as being intentional about having advocates by requesting friends or family members join them at medical appointments and mentioning their own educational backgrounds in healthcare-related fields to mitigate adverse clinical encounters due to racial discrimination. Still, some simply avoid going to the doctor at all because of the stigmatization and biased treatment they received, or heard about from others, during prior encounters with the healthcare system. These lived experiences are not only incredibly poignant, but they also offer potential explanations for persistent racial disparities in maternal health.
“We need to understand what the community experiences in order to understand how racism leads to poorer health outcomes,” says Dr. Thomas.
Since beginning her postdoc at the National Human Genome Research Institute (NHGRI), Dr. Thomas has begun to apply street race to the study of health experiences among Black women with genetic disorders, such as sickle cell disease. Dr. Thomas is working with a team of researchers in NHGRI’s Health Disparities Unit led by associate investigator Vence Bonham Jr., J.D. Together, they work to document how implicit and explicit racial bias manifests during healthcare encounters in the hopes of identifying potential areas for intervention that can improve health outcomes for historically vulnerable populations.
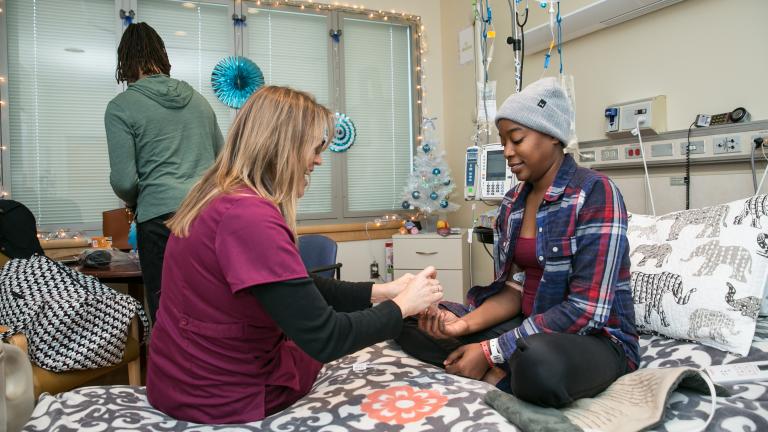
By learning more about how racial bias affects medical interactions involving Black patients, Dr. Thomas aims to improve treatment for genetic conditions, such as sickle cell disease, that are more common in Black patients than in people of other racial backgrounds.
In the future, Dr. Thomas would like to expand her research to Black families, including investigating how reproductive health disparities affect Black men and infants. However, she feels that paying special attention to the health experiences of Black mothers is key to understanding the many ways that racial discrimination affects families, from elevating stress to increasing infant mortality and many other poor health outcomes. Much of the research on maternal-child health focuses on infant health outcomes, but Dr. Thomas emphasizes that focusing on Black women’s reproductive health can improve the health of Black families as a whole.
“The birthing woman and the fetus are a pair,” Dr. Thomas explains. “In order to improve infant health outcomes, we have to incorporate the lived experience of the mother.”
Dr. Thomas recognizes that her research owes a great deal to the Black birth workers — both traditional healers as well as those clinically trained — who have played a historical role in ending unjust reproductive policies like eugenics and enforced sterilization. Although the challenges Black women face accessing healthcare have long been understood within that community, Dr. Thomas’ research gives a voice to those narratives and helps identify patterns that may help to explain persistent healthcare disparities in the U.S. She hopes her work will honor the efforts of generations of women before her, including Black midwives, doulas, and birth coaches who laid the groundwork for healthy birthing outcomes despite being historically excluded from formal healthcare systems.
“This work is not new — it’s a resurgence,” she notes. “Black birth workers have long stood on the front lines of exclusion to produce healthy babies, and we need to get back to trusting the lived experiences of Black mothers because one’s lived experience is legitimate scientific data.”
Dr. Thomas’ work illustrates that statistics on health disparities do not tell the full story of what it means to be Black in the U.S. healthcare system. By not listening to patients’ stories, researchers miss the narrative behind the numbers.
“I would love to give gratitude and deep honor to the Black women who have shared their stories with me,” Dr. Thomas says. “My work is forever indebted to them, and a desire to share their experiences keeps me going.”
Subscribe to our weekly newsletter to stay up-to-date on the latest breakthroughs in the NIH Intramural Research Program.
References:
[1] Street-Race in Reproductive Health: A Qualitative Study of the Pregnancy and Birthing Experiences among Black and Afro-Latina Women in South Florida. Thomas SP. Matern Child Health J. 2021 Jul 16. doi: 10.1007/s10995-021-03188-2.
Related Blog Posts
This page was last updated on Monday, January 29, 2024
