Rare Disease Day and the DADA2 Story
It Takes Detective Work to Diagnose Rare Diseases
Many aspects of Sherlock Holmes’s famous detective skills and eccentric mannerisms were modeled after one of Sir Arthur Conan Doyle’s medical school professors, Dr. Joseph Bell. Bell was known for using close observation to diagnose his patients’ diseases. He was reputed to be able to deduce a stranger’s occupation and recent activities based on the greeting they chose and minute details such as the dirt on their shoes. If only Sherlock Holmes or Dr. Bell could closely observe patients with rare diseases today, perhaps it would shorten the years-long diagnostic odysseys that many of them face.
At the Rare Disease Day conference, held at NIH on February 28, 2020, health-care providers, patient advocates, and patients with rare diseases shared their remarkable stories. The day was filled with talks, posters, and panel discussions, including “Shortening the Diagnostic Odyssey,” which emphasized how advances in genomics, medical informatics, and novel clinical approaches—as well as collaborations among scientists, doctors, and the community—help to make progress toward quicker diagnoses of rare diseases.

CREDIT: NCATS
Vanderbilt University physician Chip Chambers (left), who has two children with the rare disease DADA2, and NIH pediatric rheumatologist Amanda Ombrello (right), who also has a child with a rare disease, shared their stories at NIH’s Rare Disease Day in February.
“Rare stories,” about the detective work required to find such diagnoses, were highlighted at the conference. One of the remarkable stories began on a hot summer day in 1999 in Nashville, Tennessee. Two-year-old Allie Chambers was playing outside when small nodules suddenly appeared on her legs. Allie’s father—Chip Chambers, a physician at Vanderbilt University Medical Center (Nashville)—took her to a pediatric dermatologist for a medical exam, beginning her nearly 15-year-long diagnostic journey. The pediatric dermatologist suggested the girl had flea bites, but Chambers knew that wasn’t possible since the family did not have a dog.
A few months later, a skin biopsy revealed that Allie had very inflamed vessels in her skin and unusual-looking cells surrounding the vessels. At least one physician suspected that she had T-cell lymphoma, but several pathologists, including one at NIH, determined that that diagnosis was incorrect. The question was, “What did she have?”
In 2010, Allie became very sick with her liver functions going awry and her platelet count dropping. Chambers took her to the Mayo Clinic (Rochester, Minnesota) and even the doctors there couldn’t figure out what might be wrong other than diagnosing her with immunodeficiency. That same year, Allie’s younger brother Trey (age 6) developed nodules just like his sister’s.
The Mayo physicians, suspecting a hereditary link, sent samples of the siblings’ blood to Baylor College of Medicine (Houston) for then-cutting-edge whole-exome sequencing, which allows for potential disease-causing variations in the protein-coding region of any gene to be identified. Simultaneously, the Mayo doctors made a blog post about this unique case.
A doctor from Finland responded and suggested testing the children for adenosine deaminase 2 (ADA2) deficiency. At the time, there were no scientific journal articles on the disease so, in essence, the disease did not “really” exist. The Finnish doctor went on to describe that symptoms might include intermittent fevers, mottled skin discoloration, immunodeficiency, bone-marrow failure, and recurrent strokes that may begin in childhood.
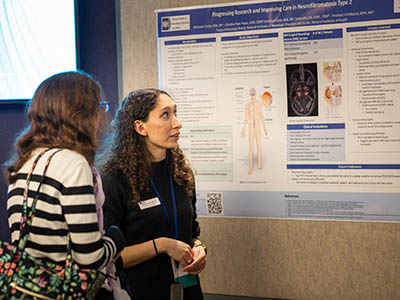
CREDIT: NCATS
Rare Disease Day was filled with talks, posters, and panel discussions. Shown: Michaela Cortes of the National Institute of Neurological Disorders and Stroke, explained her poster on “Progressing Research and Improving Care in Neurofibromatosis Type 2,” a hereditary condition associated with benign tumors that occur on the nerves for balance and hearing.
The Chambers children had most of the symptoms, but not strokes. Therefore, blood samples from the children were sent to Finland to see if they were deficient in the ADA2 enzyme. The results confirmed that their ADA2 enzymatic concentrations were virtually undetectable, which further supported the diagnosis. The children were subsequently found to have mutations in the ADA2 gene.
While the Chambers family was undergoing their diagnostic odyssey, a seemingly separate and unrelated set of odysseys were ongoing at NIH in Bethesda, Maryland. In 2002, a 2-year-old girl presented to the NIH Autoinflammatory Disease Clinic for evaluation of her fevers, strokes, and rash. At the time, she did not exhibit any of the features of known autoinflammatory diseases.
In 2011, a 6-year-old girl—also with fevers, recurrent strokes, and rash—was referred to NIH’s Undiagnosed Diseases Program. Pediatric rheumatologist Amanda Ombrello—who works for the National Human Genome Research Institute (NHGRI) and, coincidentally, followed the other little girl in clinic, and, even more ironically, also has a child with a rare disease—recognized the similarities in their cases and sent blood samples from the young girls for whole-exome sequencing. Both girls had mutations in the ADA2 gene.
In 2014, Ombrello’s group and colleagues in Jerusalem simultaneously published articles in the New England Journal of Medicine describing for the first time the disease (N Engl J Med 370:921–931, 2014; DOI:10.1056/NEJMoa13073620). NHGRI Distinguished Investigator Dan Kastner and his team named the disorder deficiency of adenosine deaminase 2, or DADA2, which can lead to inflammation in the walls of blood vessels and interfere with blood flow to the brain, resulting in strokes as well as varying immunodeficiencies and bone-marrow abnormalities (N Engl J Med 370:911–920, 2014; DOI:10.1056/NEJMoa1307361).
These diagnostic odysseys, at one time so separate, converged later in 2014 when the Chambers children’s diagnosis was confirmed by the Kastner group.
In 2016, Chambers launched the DADA2 Foundation to accelerate a search for a cure, working closely with Ombrello and Kastner. Ombrello and colleagues recently demonstrated that anti-tumor-necrosis-factor agents reduce the risk of stroke in patients with DADA2 such that none of the patients have had a stroke since going on this type of medication (N Engl J Med 380:1582–1584, 2019; DOI:10.1056/NEJMc1801927).

CREDIT: NCATS
Attendees at Rare Disease Day enjoyed the many exhibits.
The well-known-phrase, “When you hear hoofbeats, think of horses not zebras,” may not resonate well with people who have, or who are trying to diagnose, rare diseases. The quote from Sherlock Holmes, however, “When you have eliminated the impossible, whatever remains, however improbable, must be the truth” may resonate more with the rare-disease patients whose stories are far from elementary.
NIH’s Rare Disease Day is sponsored by the National Center for Advancing Translational Sciences and the NIH Clinical Center to highlight their commitment to helping people with rare disease through research, treatment development, and community empowerment. To see a videocast of Rare Disease Day, held at NIH on Friday, February 28, 2020, please visit https://videocast.nih.gov/watch=34608.
This page was last updated on Thursday, March 24, 2022
