Technology Transfer: Biologically Engineered Pacemaker
NIA Scientists Invent Biologically Engineered Pacemaker
BY DIPTADIP DATTAROY, NIDDK
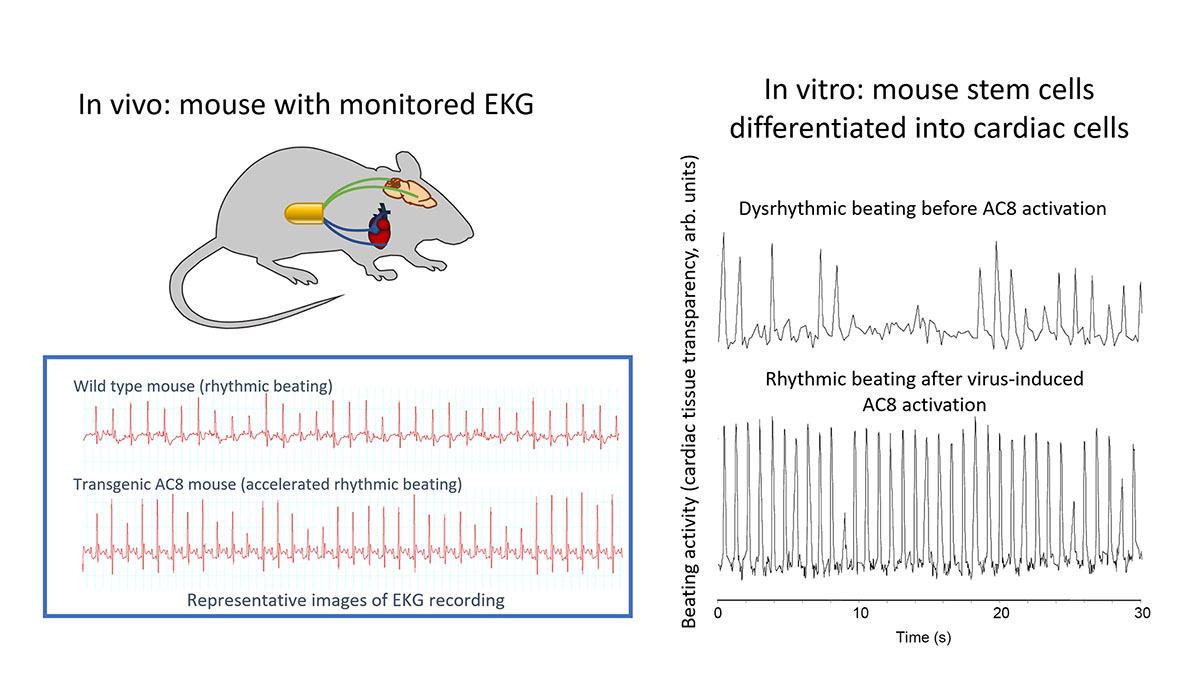
CREDIT: V. MALTSEV AND E. LAKATTA, NIA; MOUSE PICTURE: K.R. MCGRAW, NIA
NIA researchers developed a genetically engineered, cell-based biological pacemaker, which restores normal rhythmic heartbeat. Shown: (left) EKG recordings of heartbeats from a wild type mouse (top) and a transgenic AC8 mouse (bottom); (right) mouse cardiac cells showing dysrhythmic beating before AC8 activation (top) but rhythmic beating after virus-induced AC8 activation (bottom).
Staff scientist Victor Maltsev and senior investigator Edward Lakatta and colleagues at the National Institute on Aging (NIA) have invented and patented a genetically engineered biological pacemaker that may one day replace electronic pacemakers. Biological pacemakers restore normal heart rhythm in people with irregular heartbeats due to cardiovascular disease.
In the United States, about 200,000 electronic pacemakers are implanted annually; worldwide, it’s about 1 million. Most have improved the lives of recipients, but about five percent fail and require surgery or other invasive procedures to repair or replace them. In addition, electronic pacemakers have limitations such as being prone to electrode fracture, having a limited battery life, posing a risk of infection, and being subject to electromagnetic interference from other devices. These problems could be circumvented with a genetically engineered, cell-based biological pacemaker, which would not only restore normal pacing but also integrate naturally into the heart.
The heart’s natural pacemaker is a group of specialized cells residing in the sinoatrial node (SAN), which is in the upper right part of the heart’s right atrium. The SAN generates electrical impulses, action potentials, at regular intervals that signal a healthy, resting heart to pump at a rate of 60 to 70 beats per minute. The NIA investigators found that certain unique intracellular components in the SAN cells are responsible for their pacemaker functions. By introducing these cellular components into heart cells, the investigators were able to convert them into pacemaker-like cells that regulate heart rhythm.
Through a series of discoveries that started in early 2000, the NIA researchers found that the pacemaker cells express an enzyme called adenylate cyclase (AC types 1 and 8), which when activated by intracellular calcium, drives the pacemaker function and mediates heart rate (Circ Res 106:659–673, 2010). These enzymes, however, are absent in cardiac muscle cells. The NIA scientists and collaborators at University of Pittsburgh (Pittsburgh) used a genetically engineered lentivirus to deliver calcium-activated ACs (AC1 and AC8) to nonpacemaker heart cells and turned them into rhythmic and effective pacemakers.
In May 2009, the NIA inventors and their Pittsburgh collaborators filed an initial provisional patent application; a patent related to this initial application was granted in 2016 by the United States Patent and Trademark Office. This technology was tested further by scientists at Columbia University (New York) and colleagues who conducted an extensive study in dogs (Circulation 126:528–536, 2013).
At present, this biological pacemaker technology is in the early development stage and is available for licensing and co-development. The inventors aim to further develop both a genetically engineered virus—with long-term action of AC1 and AC8—and a reliable surgical method to generate robust biopacemaking in the right location of the heart. This technology may be suitable for clinical and other trials.
NIH’s intramural scientists are continually developing new drugs and medical technologies that show promise for relieving and curing human diseases. Such inventions often become available for licensing and collaboration agreements with biotech and pharmaceutical companies; many become commercially successful. To learn more, go to the Office of Technology Transfer’s website at https://www.ott.nih.gov. In addition, you can read the NIH Catalyst story on Tech Transfer (May–June 2019 issue) at https://irp.nih.gov/catalyst/v27i3/news-you-can-use-technology-transfer.
This page was last updated on Tuesday, March 29, 2022
