Research Briefs
NIDCR: SPOTLIGHT ON SJÖGREN SYNDROME
NEW EVIDENCE FOR LONG-SUSPECTED ROLE OF VIRAL INFECTIONS IN SJÖGREN SYNDROME
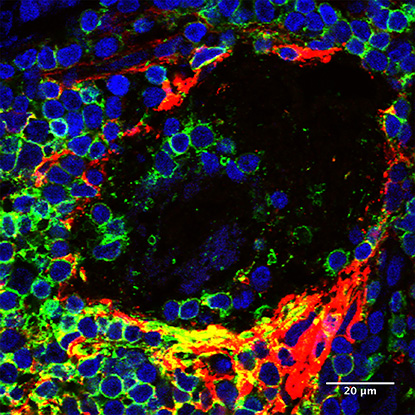
CREDIT: ILIAS ALEVIZOS, NIDCR
B lymphocytes (red and green) line the rim of a salivary duct in salivary gland tissue from a Sjögren syndrome patient.
Sjögren syndrome is an autoimmune disease in which the immune system mistakenly attacks the glands that produce tears and saliva. The causes of the syndrome have been somewhat elusive, but viral infections have long been suspected to be involved. Two studies by NIDCR researchers provide evidence for a causal relationship between infection with Epstein-Barr virus (EBV) or hepatitis delta virus (HDV) and Sjögren syndrome. These studies reveal new details on viral mechanisms at work in salivary glands and lay the foundation for developing novel therapeutic strategies for combating Sjögren syndrome.
In the first study, the researchers focused on an EBV microRNA, ebv-miR-BART13-3p, which had been found at concentrations more than 20 times as high in Sjögren patients’ salivary glands as in the salivary glands of healthy control subjects. Suspecting a role for the microRNA in the glands’ malfunction, the investigators examined its effect on the activity of salivary gland genes in cultured cells and found that it suppresses the activity of two key genes, STIM1 and AQP5. Additional experiments provided evidence for ebv-miR-BART13-3p’s inhibitory effect on STIM1 gene activity in salivary gland tissue from Sjögren syndrome patients. (NIH authors: A. Gallo, S.I. Jang, H.L. Ong, P. Perez, M. Tandon, I. Ambudkar, G. Illei, and I. Alevizos, EBioMedicine 10:216–226, 2016; http://www.ebiomedicine.com/article/S2352-3964(16)30298-5/fulltext)
In the second study, another team of NIDCR scientists observed replicating HDV in the salivary glands of 50 percent of Sjögren syndrome patients tested. When HDV proteins were expressed in the salivary glands of mice, there was a reduction in saliva production and accumulation of lymphocytes in the glands, hallmarks of the syndrome. (NIH authors: M.L. Weller, M.R. Gardener, Z.C. Bogus, M.A. Smith, E. Astorri, D.G. Michael, D.A. Michael, C. Zheng, P.D. Burbelo, Z. Lai, P.A. Wilson, W. Swaim, B. Handelman, S.A. Afione, M. Bombardieri, and J.A. Chiorini, Pathog Immun 1:12–40, 2016; https://www.paijournal.com/index.php/paijournal/article/view/72/36)
AQUAPORIN GENE THERAPY RELIEVES SYMPTOMS OF SJÖGREN SYNDROME IN MICE
A team led by NIDCR researchers has demonstrated that gene therapy with AQP1, the gene that codes for the protein aquaporin 1, restored saliva and tear flow in mice that were suffering from symptoms of Sjögren syndrome—dry mouth and dry eyes and inflamed salivary and tear glands. The syndrome is a chronic autoimmune disease that affects some 35 million people worldwide, mostly older women. Currently, there is no effective treatment for Sjögren syndrome.
Aquaporins are proteins that serve as water channels in cell membranes. In this study, the investigators introduced AQP1 into the salivary gland of mice bred to have Sjögren syndrome. The AQP1 increased water permeability of the salivary gland and enabled fluid to move constantly through ducts into the mouth, improving saliva flow in mice with dry mouth. Surprisingly, the expression of AQP1 in salivary glands also enhanced tear secretion and reduced inflammation. According to the authors, these results support the possibility of testing AQP1 gene therapy to restore saliva and tear flow in people with the syndrome. (NIH authors: Z. Lai, H. Yin, J. Cabrera-Pérez, M.C. Guimaro, S. Afione, D.G. Michael, A. Patel, W.D. Swaim, C. Zheng, and J.A. Chiorini, Proc Natl Acad Sci USA 113:5694–5699, 2016; http://www.pnas.org/content/113/20/5694.long)
NIEHS: DIFFERENCES BETWEEN ALLERGIC AND NONALLERGIC DUST-MITE PROTEINS

NIEHS scientists and others have determined what differentiates dust-mite allergens from the nonallergen proteins that dust mites produce. According to the researchers, dust-mite allergens are more chemically stable and produced in larger quantities than other dust-mite proteins. The finding that dust-mite allergens are more durable and more abundant than other dust-mite proteins supports two hypotheses about how allergenic compounds stimulate an immune response in the body.
One theory is that proteins that are more stable do not break down during the journey from the source—such as dust mites, cockroaches, and ragweed—to a person. Another possible explanation is that more-stable proteins are harder for the immune system to digest, therefore initiating signals in the body that indicate they are dangerous particles. (NIH authors: T.A. Randall, G.E. Kissling, R.E. London, and G.A. Mueller, J Allergy Clin Immunol DOI:10.1016/j.jaci.2016.08.016; http://www.jacionline.org/article/S0091-6749(16)30963-0/abstract)
NIAID, NHGRI, NIMH: GENETIC EXPLANATION FOR A FRUSTRATING SYNDROME
A team led by NIAID scientists has identified a genetic explanation for a syndrome characterized by multiple frustrating and difficult-to-treat symptoms, including dizziness and lightheadedness, skin flushing and itching, gastrointestinal complaints, chronic pain, and bone and joint problems. Some people who experience these diverse symptoms have elevated concentrations of tryptase, a protein in the blood often associated with allergic reactions. Multiple copies of TPSAB1, the gene for alpha tryptase, drive these tryptase elevations and may contribute to the symptoms, according to the study. Other studies have indicated that four to six percent of the general public has high tryptase concentrations. Although not all of these people experience symptoms, many do, raising the possibility that this mildly prevalent trait in some cases drives the symptoms, although how it does so remains unclear.
Previously, NIAID researchers had observed that a combination of chronic and sometimes debilitating symptoms, such as hives, irritable bowel syndrome, and overly flexible joints, runs in some families and is associated with high tryptase concentrations. Although more research is needed to understand how elevated tryptase contributes to this constellation of symptoms, this study helps set the stage for future advances in diagnosis and treatment. The scientists are also planning to develop strategies to block alpha tryptase, which potentially could ease the health problems associated with additional copies of the gene. (NIAID authors: J.J. Lyons, X. Yu, A. Jamil, Y. Bai, Y. Liu, M.P. O'Connell, C. Nelson, T. DiMaggio, R.J. Carlson, S. Agama, T.M. Wilson, S. Tucker, K.D. Stone, D.D. Metcalfe, J.D. Milner, M. Zhao, R.J. Hohman, H. Matthews, A.J. Oler, and Y. Zhang; NHGRI authors: K.L. Lewis, C. Hong, and L.G. Biesecker; NIMH author: M. Pao; Nat Genet DOI:10.1038/ng.3696, 2016; http://www.nature.com/ng/journal/vaop/ncurrent/full/ng.3696.html)
NIDDK: WEIGHT LOSS LEADS TO STRONG INCREASE IN APPETITE
Analysis of a trial that used the drug canagliflozin found that as people lost weight, their appetite increased proportionately, leading to the consumption of more calories and a leveling off of weight loss. The findings provide the first measurement in people of how strongly appetite counters weight loss as part of the body’s feedback-control system regulating weight. A team led by NIDDK investigators analyzed data from a year-long, placebo-controlled, double-blind trial in people with type 2 diabetes who could eat and drink without restriction. Of the 242 participants, 153 received canagliflozin, a drug that caused a substantial increase in the amount of glucose excreted in their urine. Those people were not directly aware of that calorie loss, which caused a gradual decrease in weight averaging about eight pounds.
The team used a validated math model to calculate the changes in the amount of calories consumed during the study. They found no long-term calorie-intake changes in the 89 people who got a placebo. However, for every pound of lost weight, the people treated with canagliflozin consumed about 50 calories per day more than they were eating before the study. This increase in appetite and calorie intake led to slowing of weight loss after about six months. Findings from the analyses suggest that persistent effort is required to avoid weight regain. (NIH authors: A. Sanghvi and K.D. Hall, Obesity DOI:http://dx.doi.org/10.1101/051045; http://biorxiv.org/content/early/2016/04/29/051045)
NIAID: ZMAPP HOLDS PROMISE AS EBOLA TREATMENT
A randomized, controlled clinical trial to evaluate the experimental Ebola treatment ZMapp found it to be safe and well-tolerated. But, because of the waning Ebola epidemic, the study enrolled too few people to determine definitively whether it is a better treatment for Ebola virus disease (EVD) than the best available standard of care alone—providing intravenous fluids, balancing electrolytes needed to maintain bodily functions, and maintaining healthy oxygen and blood pressure levels. ZMapp is designed to prevent the progression of EVD by targeting the main surface protein of the Ebola virus. Earlier studies in nonhuman primates demonstrated that ZMapp had strong antiviral activity and prevented death when administered as late as five days after experimental infection with Zaire ebolavirus.
The trial enrolled 72 participants (average age was 24) with confirmed Ebola virus infection from March 2015 through November 2015. The participants came from Sierra Leone (54), Guinea (12), Liberia (five), and the United States (one, a health-care worker evacuated from Sierra Leone). Slightly more than half of the study participants were women. The study sought to determine whether the experimental drug ZMapp plus the optimized standard of care for treating EVD was superior to the optimized standard of care alone in reducing deaths caused by EVD. Those randomly assigned to the ZMapp arm also received three intravenous infusions of ZMapp administered three days apart. (NIH authors: R.T. Davey, Jr., L. Dodd, M.A. Proschan, J. Tierney, H.C. Lane, and A.S. Fauci, N Engl J Med 375:1448–1456, 2016; http://www.nejm.org/doi/full/10.1056/NEJMoa1604330)
NICHD: MORNING SICKNESS LINKED TO LOWER RISK OF PREGNANCY LOSS

CREDIT: NIDDK
Nausea and vomiting during pregnancy is associated with a lower risk of miscarriage in pregnant women, according to a new analysis by NICHD researchers and others. The cause of morning sickness is not known, but scientists have proposed that it protects the fetus against toxins and disease-causing organisms in foods and beverages. For their study, the researchers analyzed data from the Effects of Aspirin in Gestation and Reproduction (EAGeR) trial, which tested whether taking daily low-dose aspirin prevented women who had experienced one or two previous pregnancy losses from experiencing a future loss.
The authors looked at data from 797 women who had positive pregnancy tests, with 188 pregnancies ending in loss. By the eighth week of pregnancy, 57.3 percent of the women reported experiencing nausea, and 26.6 percent reported nausea with vomiting. The researchers found that these women were 50 to 75 percent less likely to experience a pregnancy loss than those who had not experienced nausea alone or nausea accompanied by vomiting. (NIH authors: S.N. Hinkle, S.L. Mumford, K.L. Grantz, E.M. Mitchell, L.A. Sjaarda, R.G. Radin, N.J. Perkins, and E.F. Schisterman, JAMA Intern Med DOI:10.1001/jamainternmed.2016.5641; http://jamanetwork.com/journals/jamainternalmedicine/article-abstract/2553283)
NICHD: DEPRESSION IN EARLY PREGNANCY LINKED TO GESTATIONAL DIABETES
Researchers at NICHD have discovered a two-way link between depression and gestational diabetes (diabetes occurring only during pregnancy). Women who reported feeling depressed during the first two trimesters of pregnancy were nearly twice as likely to develop gestational diabetes, according to an analysis of pregnancy records. Conversely, a separate analysis found that women who developed gestational diabetes were more likely to report postpartum depression six weeks after giving birth than a similar group of women who did not develop gestational diabetes. The researchers analyzed pregnancy records from the NICHD Fetal Growth Studies-Singleton Cohort, which tracked the progress of thousands of pregnancies, to understand the patterns of fetal growth. The study enrolled 2,334 nonobese and 468 obese women in weeks eight to 13 of pregnancy. The women responded to questionnaires on symptoms of depression when they enrolled in the study, again between the 16th and 22nd week of pregnancy, and then six weeks after giving birth. The researchers also reviewed the women’s records to identify who had developed gestational diabetes.
Although obesity increases the risk for gestational diabetes, nonobese women with high depression scores had nearly triple the risk for gestational diabetes than the other women in the study. Depression did not appear to increase the risk for gestational diabetes among obese women. The researchers also found a higher risk for postpartum depression among the women who had gestational diabetes. Of the women who developed gestational diabetes, nearly 15 percent experienced depressive symptoms after birth, which was more than four times the rate of women who had not had gestational diabetes.
The study was not able to prove a cause-and-effect relationship between symptoms of depression and gestational diabetes, according to the researchers. However, earlier studies showed that depression is associated with impaired glucose metabolism that may lead to higher blood glucose concentrations. Similarly, high blood glucose concentrations may lead to inflammation and hormonal and other changes that could lead to symptoms of depression. (NICHD authors: S.N. Hinkle, G.M. Buck Louis, S. Rawal, Y. Zhu, P.S. Albert, and C. Zhang; Diabetologia DOI:10.1007/s00125-016-4086-1; http://link.springer.com/article/10.1007/s00125-016-4086-1)
NINDS, NCCIH, CC: “SIXTH SENSE” MAY BE MORE THAN JUST A FEELING

CREDIT: BÖNNEMANN LAB, NINDS
An NIH Study shows that two young patients with a mutation in the PIEZO2 gene have problems with touch and proprioception, or body awareness.
With the help of two young patients—one nine and the other 19—with a unique neurological disorder, an initial study by NIH scientists suggests that a gene called PIEZO2 controls specific aspects of human touch and proprioception, a “sixth sense” describing the awareness of one’s body in space. Mutations in the gene caused the two to have movement and balance problems and the loss of some forms of touch. Despite their difficulties, they both appeared to cope with these challenges by relying heavily on vision and other senses. The two patients have difficulties walking; have hip, finger, and foot deformities; and have abnormally curved spines diagnosed as progressive scoliosis.
Further examinations at the NIH Clinical Center suggested the young patients lacked body awareness. Blindfolding them made walking extremely difficult, causing them to stagger and stumble from side to side while assistants prevented them from falling. It was also harder for them, when blindfolded, to reach for an object in front of their faces compared with unaffected volunteers, and they could not guess the direction their joints were being moved. The patients were also less sensitive to certain forms of touch. Brain scans of one patient showed no response when the palm of her hand was brushed. Nevertheless, the patients could feel other forms of touch.
Despite these differences, the patients’ nervous systems appeared to be developing normally. They were able to feel pain, itch, and temperature normally; the nerves in their limbs conducted electricity rapidly; and their brains and cognitive abilities were similar to the control subjects of their age. (NCCIH authors: A.T. Chesler, M. Szczot, M. Čeko, and C. Laubacher; NINDS authors: D. Bharucha-Goebel, S. Donkervoort, L. H. Hayes, D. Nguyen, A.R. Foley, C.E. Le Pichon, and C.G. Bönnemann; CC authors: K. Alter, C. Zampieri, and C. Stanley; N Engl J Med 375:1355–1364, 2016; http://www.nejm.org/doi/full/10.1056/NEJMoa1602812)
This page was last updated on Tuesday, April 12, 2022
