Research Briefs
NIAID, CC: INVESTIGATIONAL MALARIA VACCINE FOUND SAFE AND PROTECTIVE

THOMAS WELLEMS, NIAID
The female Anopheles gambiae mosquito can transmit malaria parasites as she takes a blood meal. NIH researchers recently tested an investigational malaria vaccine and found it to be safe and protective.
An investigational malaria vaccine has been found to be safe, to generate an immune response, and to offer protection against malaria infection in healthy adults, according to the results of an early-stage clinical trial conducted at NIH. The vaccine, known as the PfSPZ vaccine, was developed by scientists at Sanaria Inc. (Rockville, Md.) The PfSPZ vaccine is composed of live but weakened sporozoites of the species Plasmodium falciparum, the most deadly of the malaria-causing parasites.
The phase 1 trial, which took place at the NIH Clinical Center, received informed consent from and enrolled 57 healthy adult volunteers ages 18 to 45 years who had never had malaria. Of these, 40 participants received the vaccine and 17 did not. To evaluate the vaccine’s safety, researchers split vaccinees into groups receiving two to six intravenous doses of PfSPZ vaccine at increasing dosages. After vaccination, participants were monitored closely for seven days. Based on blood measurements, researchers found that participants who received a higher total dosage of PfSPZ vaccine generated more antibodies against malaria and more T cells specific to the vaccine.
To evaluate whether and how well the PfSPZ vaccine prevented malaria infection, researchers exposed all the participants to bites by five mosquitoes carrying the P. falciparum strain from which the PfSPZ vaccine was derived. The researchers found that higher dosages of PfSPZ vaccine were associated with protection against malaria infection. Only three of the 15 participants who received higher dosages of the vaccine became infected, compared with 16 of 17 participants in the lower-dosage group. Among the 12 participants who received no vaccine, 11 participants became infected after mosquito challenge.
An important challenge in the continued development of PfSPZ vaccine is that the vaccine currently is administered intravenously—a rare delivery route for vaccines. Previous studies at lower doses showed that the more common intradermal (into the skin) and subcutaneous (under the skin) routes did not yield as strong an immune response as the intravenous route. Several follow-up studies are planned, including research to evaluate the vaccine’s different dose schedules, possible protection against other Plasmodium strains, and the durability of protection. The researchers may also evaluate whether higher doses administered subcutaneously or intradermally provide the same protection as found in this study. (NIH authors: R.A. Seder and others, Science DOI:10.1126/science.1241800)
NCI: HOW CANCER CHROMOSOME ABNORMALITIES FORM IN LIVING CELLS
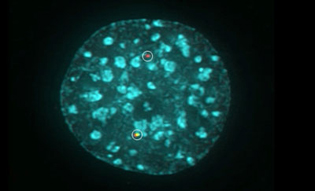
A chromosome translocation visualized by breaks marked with differently colored fluorescent proteins (green, red). DNA is stained cyan.
For the first time, scientists have directly observed events that lead to the formation of chromosome abnormalities, called translocations, often found in cancer cells. Despite many years of research, just exactly how translocations form in a cell has remained a mystery. To better understand this process, NCI researchers created an experimental system in which they induced breaks in the DNA of different chromosomes in living cells. Using sophisticated imaging technology, they were then able to watch as the broken ends of the chromosomes reattached correctly or incorrectly inside the cells. The scientists were able to demonstrate that translocations can occur within hours of DNA breaks and that their formation is independent of when the breaks happen during the cell-division cycle. (NCI authors: V. Roukos, T.C. Voss, C.K. Schmidt, D. Wangsa, and T. Misteli, Science 341:660–664, 2013)
NCI: STUDY LINKS HODGKIN LYMPHOMA TREATMENT TO POSSIBLE RISK OF STOMACH CANCER
Hodgkin lymphoma survivors who received certain radiation and chemotherapy regimens are at increased risk of later developing stomach cancer, according to a recent study by NCI scientists. Although the cure rate for Hodgkin lymphoma is high (the five-year survival rate from 2003 to 2009 was 88 percent), there is a risk of developing secondary malignancies, such as breast cancer, lung cancer, and stomach cancer. Past studies linked Hodgkin lymphoma radiation and chemotherapy treatments with stomach cancer risk, but those studies were limited in scope.
The NCI researchers analyzed data from the Netherlands, Denmark, Finland, Norway, Sweden, the United States, and Canada. Their analyses included nearly 20,000 survivors of the disease who were diagnosed between 1953 and 2003. Of 17,477 Hodgkin lymphoma cases examined, the researchers identified 89 survivors who later developed stomach cancer. The researchers showed that the risk of stomach cancer increased with increasing doses of radiation to the stomach. Patients who received the highest radiation doses had a risk of stomach cancer nearly threefold that of patients who received the lowest doses. Further, the risks associated with radiation were even higher for survivors who also received the alkylating agent procarbazine, a type of chemotherapy known to damage DNA. Stomach cancer risks depended highly on the doses of both radiation and procarbazine. This study is the first to provide clear evidence of a strong interaction between chemotherapy and radiotherapy on risk of later stomach cancer. (NCI authors: L.M. Morton, G M. Dores, R.E. Curtis, E.S. Gilbert, R.A. Kleinerman, and J.F. Fraumeni, Jr., J Clin Oncol DOI:10.1200/JCO.2013.50.6832)
NHGRI, NIDDK: THERAPY THAT MAY CURB KIDNEY DETERIORATION IN PATIENTS WITH RARE DISORDER
A team led by NIH researchers has overcome a major biological hurdle in an effort to find improved treatments for patients with a rare disease called methylmalonic acidemia (MMA). Using genetically engineered mice, the team identified a set of biomarkers of kidney damage—a hallmark of the disorder—and demonstrated that antioxidant therapy protected kidney function in the mice. MMA, which involves loss of function of a metabolic pathway that moderates concentrations of methylmalonic acid, damages the kidneys. It affects as many as one in 67,000 children born in the United States. The most common therapy is a restrictive diet, but doctors must resort to renal dialysis or kidney transplantation when the disease progresses. People with MMA also suffer from severe metabolic instability, failure to thrive, intellectual and physical disabilities, pancreatitis, anemia, seizures, vision loss, and strokes. NHGRI researchers validated the same biomarkers in 46 patients with MMA seen at the NIH Clinical Center. The discovery paves the way for use of antioxidant therapy in a clinical trial for people with MMA. It also illustrates the mechanisms by which dysfunction of mitochondria plays a role in kidney disease. Mitochondrial dysfunction is a factor not only in rare disorders, such as MMA, but also in a wide variety of common conditions, such as obesity, diabetes, and cancer. (NIH authors: I. Manolia, J.R. Sysol, L. Li, P. Houillier, C. Wang, P.M. Zerfas, J.L. Sloan, R.J. Chandler, A.G. Elkahloun, V. Hoffmann, J. Schnermann, and C.P. Venditti, Proc Natl Acad Sci U S A 110:13552–13557, 2013)
NIA: DIABETES DRUG IMPROVES HEALTH AND EXTENDS LIFESPAN IN MICE
Long-term treatment with the type 2 diabetes drug metformin improves health and longevity of male mice when started at middle age, reported an international team of scientists led by NIA researchers. The study, which tested two doses of the drug (0.1 percent and 1 percent metformin) in the male mice, found the higher dose to be toxic in the animals. Scientists emphasized that considerably more research is needed before the implications of metformin for healthy aging are known for humans. Prescribed since the 1960s to treat type 2 diabetes, metformin is known to enhance insulin sensitivity, prompting the conversion of glucose to energy and preventing its build-up in the liver. It also reduces risk of health problems associated with metabolic syndrome, a condition characterized by an increased chance for heart disease and stroke, and type 2 diabetes. The study offers evidence that metformin may provide some of the same positive effects as calorie restriction.
A battery of tests performed with male mice taking 0.1 percent, 1 percent, or no metformin starting at middle age revealed a clear health benefit of the 0.1 percent treatment. The mice on this dose had improved general fitness and weighed less than the control group mice, despite consuming more calories. Metformin increased their use of fat for energy. Mice on metformin tended to preserve body weight with age, a characteristic associated with increased survival in other studies. Not surprisingly, metformin prevented the onset of metabolic syndrome. (NIA authors: A. Martin-Montalvo, E.M. Mercken, S.J. Mitchell, H.H. Palacios, T.M. Ward, R.K. Minor, M. Bernier, Y. Yu, and R. de Cabo, Nat Commun 4:2192, 2013)
NIAAA, NIDDK: ENDOCANNABINOIDS TRIGGER INFLAMMATION THAT LEADS TO DIABETES
NIAAA and NIDDK researchers and scientists from two other institutions have clarified in rodent and test-tube experiments the role that inflammation plays in type 2 diabetes, and they have revealed a possible molecular target for treating the disease. The researchers said that some natural messenger chemicals in the body are involved in an inflammatory process that can kill the beta cells—which store and release insulin—in the pancreas.
Endocannabinoids are natural messengers in the body that help regulate many biological functions. They are chemically similar to the active compound in marijuana. Recent studies have tied endocannabinoids to the metabolic problems that lead to diabetes. Researchers also have recognized that inflammation appears to play an important role in the pathology of diabetes.
Working with a strain of genetically obese rats that serve as a model for human type 2 diabetes, the researchers demonstrated that endocannabinoid activation of macrophages in the pancreas leads to activation of a protein complex within macrophages called the Nlrp3 inflammasome. The inflammasome in turn releases molecules that cause the death of pancreatic beta cells and the progression of type 2 diabetes. Most notably, the researchers showed that by selectively blocking the expression of cannabinoid receptors on macrophages, they could protect and restore beta cell function in the genetically obese rats, which delayed the development and reduced the severity of their diabetes. The authors concluded that the findings point to a key role in type 2 diabetes for endocannabinoid-induced inflammasome activation in macrophages, and they identify cannabinoid receptors on macrophages as a new therapeutic target. [NIH authors: T. Jourdan, G. Godlewski, R. Cinar, A. Bertola, G. Szanda, J. Liu, J. Tam, T. Han, B. Mukhopadhyay, M.C. Skarulis, and G. Kunos, Nat Med DOI:10.1038/nm.3265)
NIAAA: CHRONIC ALCOHOL USE SHIFTS BRAIN’S CONTROL OF BEHAVIOR
Chronic alcohol exposure leads to brain adaptations that shift behavior control away from an area of the brain involved in complex decision-making and toward a region associated with habit formation, according to a new study conducted in mice by NIAAA scientists. The findings provide insight into how excessive drinking affects learning and behavioral control at the neural level. The brain’s prefrontal cortex is involved in decision-making and controlling emotion, whereas the dorsal striatum is thought to play a key role in motivation and habit formation. Past studies showed that alcohol-dependent individuals have problems with skills mediated by the prefrontal cortex such as impulse control. These same individuals often show exaggerated neural response in the dorsal striatum to alcohol-related cues.
The researchers measured changes in the brains of mice that were chronically exposed to alcohol vapors and found profound changes in the dorsal striatum, including the expansion of neuronal dendrites. Such changes are also seen with chronic exposure to drugs such as amphetamine. These structural changes were associated with changes in synaptic plasticity and reduced activity of endocannabinoid receptors, which are part of a signaling system that may play a role in sensation, mood, and memory. The findings suggest that drug abuse doesn’t simply impair brain functions, but instead produces a complex set of adaptations that tamp down the function of some brain regions while enhancing the function of others. (NIAAA authors: L. DePoy, R. Daut, J.L. Brigman, K. MacPherson, N. Crowley, O. Gunduz-Cinar, C.L. Pickens, R. Cinar, G. Kunos, D.M. Lonvinger, M.C. Camp, and A. Holmes, Proc Natl Acad Sci U S A DOI:10.1073/pnas.1308198110)
NIEHS, NCI: 3-D IMAGES SHOW FLAME RETARDANTS CAN MIMIC ESTROGENS
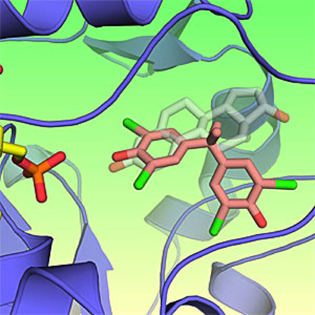
The brominated flame retardant TBBPA is shown, in this 3-D image, binding to the active site of an estrogen metabolizing enzyme (pink), interfering with the body’s natural release of estrogen (transparent gray).
By determining the three-dimensional (3-D) structure of proteins at the atomic level, NIH researchers have discovered how some commonly used flame retardants, called brominated flame retardants (BFRs), can mimic estrogen hormones and possibly disrupt the body’s endocrine system. They looked closely at one of the most widely used BFRs, tetrabromobisphenol A (TBBPA). The researchers used X-ray crystallography to build a 3-D model of the protein binding to flame retardants. They examined how the binding of TBBPA and a metabolite, or derivative, of another flame retardant called tetrabromodiphenyl ether compared with the binding of estradiol, a naturally occurring estrogen, to estrogen sulfotransferase. The researchers hope the findings will be used by companies to develop safer alternatives to current flame retardants. (NIH authors: R.A. Gosavi, G.A. Knudsen, L.S. Birnbaum, L.C. Pedersen, Environ Health Perspect DOI:10.1289/ehp.1306902)
NINDS: NIH RESEARCHERS DISCOVER HOW BRAIN CELLS CHANGE THEIR TUNE
SHENG LAB, NINDS
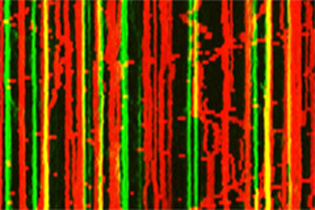
Mitochondria Take to the Dance Floor – NIH researchers used advanced microscopic techniques to watch mitochondria dance around and tune nerve cell voices. This kymograph describes their dynamic steps.
NINDS researchers recently showed that brief bursts of chemical energy coming from the mitochondria may fine-tune brain cell communication. Neurotransmitters are sent from tiny protrusions on nerve cells, called presynaptic boutons, which are aligned, like beads on a string, on axons. In this study, the researchers showed that mitochondria—which can rapidly move along axons, dancing from one bouton to another—may control the strength of the signals sent from boutons.
The scientists used advanced microscopic techniques to watch mitochondria move among boutons while the boutons released neurotransmitters. They found that boutons sent consistent signals when mitochondria were nearby. Surprisingly, when mitochondria were missing or moving away from boutons, the signal strength fluctuated. The results suggested that the presence of stationary mitochondria at synapses controls the stability of the nerve signal strength.
To test this idea further, the researchers manipulated mitochondrial movement in axons by changing concentrations of syntaphilin, a protein that helps anchor mitochondria to the nerve cell’s skeleton, which is found inside axons. Removal of syntaphilin resulted in faster-moving mitochondria, and electrical recordings of these neurons showed that the signals they sent fluctuated greatly. Conversely, elevating syntaphilin concentrations in nerve cells arrested mitochondrial movement and resulted in boutons that sent signals of the same strength.
The researchers also found that using the drug oligomycin to block production of adenosine-5'-triphosphate in mitochondria reduced the size of the signals boutons sent even if a mitochondrion was nearby. Problems with mitochondrial energy production and movement throughout nerve cells have been implicated in Alzheimer disease, Parkinson disease, amyotrophic lateral sclerosis, and other major neurodegenerative disorders. The researchers think these results will ultimately help scientists understand how mitochondrial problems can lead to disorders in brain cell communication. (NINDS authors: T. Sun, H. Quiao, P-Y. Pan, Y. Chen, Z-H. Sheng, Cell Rep 4:413–419, 2013)
To see a video of the nerve cell power plant dancing, go to https://youtu.be/qbm5jXCL3ZA.
HELA GENOME ACCESS BROKERED BY COLLINS AND NIH
NIH announced a privacy agreement with the family of the late Henrietta Lacks to allow for the limited use of genomic sequence data from cells derived from her tumor, commonly known as HeLa cells. HeLa cells are the most widely used human cell line in existence today and have been used in the development of modern vaccines, cancer treatments, in vitro fertilization techniques, and other medical advances. Lacks died of cervical cancer in 1951, before scientists were required to get permission to use a patient’s cells in research.
This spring, German scientists sequenced the genome of a HeLa cell line and posted the data in a public database. The data had the potential to reveal private genetic information about the Lacks family. NIH Director Francis Collins and NIH Deputy Director for Science, Outreach, and Policy Kathy Hudson met with members of the Lacks family to discuss the research. They settled on an agreement for use of HeLa data: Published genomes will be stored in an NIH-controlled database, accessed only by researchers who agree to terms of use defined by a panel that includes Lacks family members. Collins noted that the new policy allows for public data sharing while showing the respect that NIH and scientists have for the contributions of the Lacks family. (K.L. Hudson and F.S. Collins, Nature 500:141–142, 2013)
PUBLISH AND FLOURISH
It’s difficult to get official numbers, but if you do a search via PubMed, you will see that NIH researchers are authoring approximately 500 peer-reviewed journal articles each month. Some of these articles are featured on flat-screen monitors at the Clinical Center. Some are featured in the “Hot Topics” section of the relatively new Intramural Research Program (IRP) Web site at https://irp.nih.gov/news-and-events/hot-topics.
It’s a fantastic number, considering we have about 1,000 labs at the NIH. Now the journal Nature has provided some documentation. According to the Nature Publishing Index 2012 (http://www.natureasia.com/en/publishing-index/global/), the NIH ranks #6 in the number of papers published in the Nature family of journals. Only #6, you ask? Well, of course, NIH isn’t competitive in physics, astronomy, engineering, and many other fields dominated by the top five on the list: Harvard, Stanford, Max Planck, Massachusetts Institute of Technology, and the French National Centre for Scientific Research (CNRS).
Also, the CNRS and Max Planck organizations represent a good deal of their nation’s investment in research; their rankings are equivalent to counting all NIH-supported research (extramural and intramural) with a little NSF and NASA thrown into the mix.
Nevertheless, if you break down the Nature numbers, the NIH IRP ranked #2 for Nature Genetics, Nature Neuroscience, Nature Medicine, and Nature Immunology; #3 for Nature Structural and Molecular Biology; and #5 for Nature Chemical Biology. Not bad when you also consider that the Nature journals aren’t necessarily our preferred venue for publication.
The bottom line is that we are a productive bunch, and I hope we can keep up that productivity and maintain our rankings through the inevitable downsizing that will occur if budgets remain flat or additional cuts are mandated.
NIH DIRECTOR’S CHALLENGE INNOVATION AWARDS
The NIH Director’s Challenge Innovation Awards program is supporting 10 intramural projects for research on antibacterial drug resistance. The program, which provides seed money to stimulate innovative, high-impact research, gives priority to applications that involve collaborations among PIs from multiple NIH Institutes and Centers. This year, $750,000 is supporting the projects, with awards ranging from $45,000 to $100,000 per year. The next competition is scheduled for FY2015.
The following were awarded funding for FY2013 and FY2014:
Anirban Banerjee (NICHD) with researchers from NIAID: Structural and Chemical Biology Approach to Targeting MraY—an Integral Membrane Enzyme in the Bacterial Peptidoglycan Biosynthesis Pathway
Robert Danner (CC) with researchers from NCI and NHGRI: Engineering a Multivalent Bacteriophage Targeting KPC+ K. pneumoniae
John Barrett (NHLBI) with researchers from CC and NIAID: Th17 Cells for Treatment of Carbapenem Resistant Klebsiella pneumoniae
Yasmine Belkaid (NIAID) with researchers from NCI, NHGRI, and NIAID: Role of the Microbiota in KPC-producing Klebsiella Pneumonia Infection
Karen Frank (CC) with researchers from NCI and NHGRI: Carbapenemase blaKPC Horizontal Transfer between Enterobacteriacae
Julie Segre (NHGRI) with researchers from CC: Microbiome Studies of CC Patients at Risk for Multidrug-Resistant Bacteria
Susan Buchanon (NIDDK) with researchers from NCI: Klebsiella Capsule as a Target for Novel Antibiotics: Genetics, Structure/function and Small Molecule Screens
Adrian Ferre D’Amare (NHLBI) with researchers from NCI: High-throughput Discovery of Antibiotics Against Bacterial Riboswitches
Matthias Machner (NICHD) with researchers from NCATS: Discovering “Smart” Drugs That Target Only Pathogenic Bacteria
Roger Woodgate (NICHD) with researchers from NCATS: Inhibitors of LexA/DinR Cleavage Combat Evolution of Antibiotic Resistance
For more information, visit http://sigs.nih.gov/challenge/Pages/FundedProjects.aspx.
This page was last updated on Thursday, April 28, 2022
