Robotic Arms
Physical Therapists of the Future?
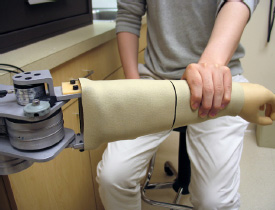
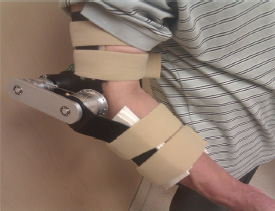
Photo: Hyung Park and Jonghyun Kim, CC
NIH researchers have developed tele-rehabilitation robots that can treat weakened elbow joints. The clinician manipulates the haptic mannequin device (top), which sends signals from a computer via the Internet to remotely maneuver the wearable stretching device (bottom) worn by the patient. The patient device sends signals that make the mannequin arm move and feel just like the patient’s.
In a small room tucked away on the first floor of the Clinical Center (CC), NIH scientists are building robots. But don’t expect to see armies of cyborg clinicians marching through the hallways any time soon. These robots are mechanical devices that provide physical therapy assessment and training to patients whose muscles have been weakened by cerebral palsy, traumatic brain injury (TBI), or other neurological disorders. The machines can even be operated remotely. For example, a clinician in an office could control a robot that is providing therapy to a patient at home.
“We are coming to a Renaissance in robotics,” said Leighton Chan, chief of the CC’s Rehabilitation Medicine Department. They “can play a huge role” in physical therapy.
Guided by computers, these first-of-their-kind rehabilitation robots can help patients by assessing muscle-related tasks or training weakened muscles to regain their strength. Hyung-Soon Park, a staff scientist in the CC’s Functional and Applied Biomechanics Section (FABS), leads the design and development of the robots. FABS chief Diane Damiano works with patients and develops clinical questions that robotics technology can address.
Usually a patient who needs physical therapy must come to a clinical facility. But Park is developing a tele-rehabilitation system that can remotely assess a patient’s condition and provide treatment. Patients could be helped without ever having to leave home.
Park’s lab developed two robotic mechanisms that work together to rehabilitate the elbow joint. The first, which resembles a human arm, is a haptic mannequin device (HMD) that relies on the sense of touch. It is attached to a computer in the clinician’s office. The second is a mechanical arm brace, called a wearable stretching device (WSD). The patient wears the WSD and can be at home or in some other location but must be near a computer that is connected to the Internet.
Patients who suffer from involuntary muscle spasms caused by neurological impairments are one group that could benefit from this robotic tele-rehabilitation system. Normally a clinician has to have physical contact with a patient to feel the muscles, diagnose problems, and provide physical therapy. But with the HMD-WSD setup, the clinician moves the HMD mechanical arm; a signal travels via the Internet to the patient; the WSD arm brace that the patient is wearing mimics the movement and stretches the muscles. The WSD records muscle resistance and relays the information back to the HMD so it moves and feels just like the patient’s arm. The two devices talk to each other, sharing information instantaneously as if the patient and the clinician are sitting in the same room.
Clinical trials with the HMD-WSD system are expected to begin in the near future. After the system has been perfected, Park hopes to develop devices that focus on the knee, ankle, wrist, and shoulder.
Whether patients are being clinically managed or participating in clinical trials, “you could test people remotely all over the country and monitor them at home,” said Damiano.
The robotic arm can also be used as a tool to standardize medical assessments and to train clinicians who want to improve their physical therapy skills. It is programmed using patient data and can provide realistic, consistent movements, including imitating spasticity (muscle stiffness) and contracture (a permanent shortening of the muscle).
Park and Damiano are also developing other robotic devices. Their robotic leg may help to eliminate crouch gait in children with cerebral palsy. Crouch gait causes a child’s knees to flex and turn inward, makes walking difficult and exhausting, and often leads to the permanent use of a walking aid. The robotic device could improve leg strength and help children with cerebral palsy to stand more upright.
The researchers have also developed a self-paced treadmill that is helping patients who have suffered a TBI relearn how to walk. The machine allows patients to choose their speed via sensors that are attached to the body and linked to a computer program developed by FABS. The treadmill faces a large screen onto which a virtual world is projected. Patients walk through the mock terrain, turn corners, and even navigate crowded hallways, actions that can be difficult for someone who has suffered a TBI.
“If your brain is engaged, the response to training [is] greater,” said Damiano. The system also “gives you practice in a more real-world setting.”
Who knows what the NIH rehab robotics team will come up with next?
To learn more about FABS, visit http://clinicalcenter.nih.gov/rmd/fab.
This page was last updated on Monday, May 2, 2022
