Dual role discovered for molecule involved in autoimmune eye disease
IL-17, known for driving inflammation, also puts on the brakes, NIH scientists report
The inflammatory molecule interleukin-17A (IL-17A) triggers immune cells that in turn reduce IL-17A’s pro-inflammatory activity, according to a study by National Eye Institute (NEI) researchers. In models of autoimmune diseases of the eye and brain, blocking IL-17A increased the presence of other inflammatory molecules produced by Th17 cells, immune cells that produce IL-17A and are involved in neuroinflammation. The finding could explain why IL-17-targeted treatments for conditions like the eye disease autoimmune uveitis and multiple sclerosis (MS) have failed. A report on the findings was published in Immunity. NEI is part of the National Institutes of Health.
In autoimmune uveitis, immune cells become abnormally activated and begin to destroy healthy cells, including light-sensing photoreceptors and neurons. A key immune cell involved in this response is the Th17 lymphocyte, which produces several pro-inflammatory molecules known as cytokines. A hallmark of Th17 cells is the ability to produce IL-17A, which attracts immune cells called neutrophils that can damage tissue. Nevertheless, multiple clinical trials of drugs that block IL-17A have failed to help people with autoimmune uveitis or MS.
“IL-17 is the prototypical inflammatory immune molecule blamed for autoimmunity in the neuro-retina and the brain, but there’s been some controversy about the role it plays,” said Rachel Caspi, Ph.D., chief of the Laboratory of Immunology at NEI and senior author of the study. “In our model of autoimmune uveitis, we noticed that without IL-17, the amount of tissue damage unexpectedly stayed the same and we had higher levels of other inflammatory molecules.”
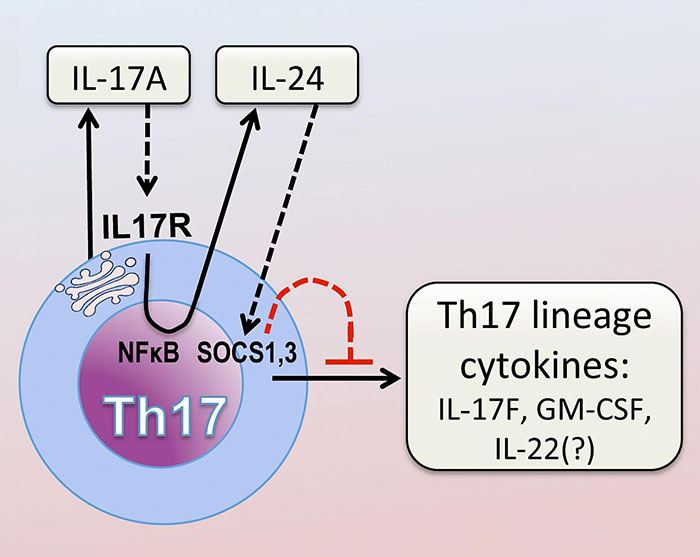
After activation through its T-cell receptor, Th17 cells produce IL-17A, which binds to its own receptor on the Th17 cell. This activates the NFκB pathway. NFκB drives production of IL-24, which in turn suppresses the Th17 cytokine program via SOCS1 and 3.
This page was last updated on Friday, January 21, 2022