An Eye to a Cure
Anand Swaroop aims to treat retinal diseases with cell-based therapies.


Postdoctoral Fellow Winnette McIntosh Ambrose brings an engineering background to the Swaroop laboratory
“If we want to repair the degenerating retina,” explains Anand Swaroop, Ph.D., “we need to know how to make specific cell types. Our focus has been on photoreceptors because, in the majority of retinal diseases, it is the photoreceptors that die.”
For over 20 years, Swaroop’s laboratory has studied retinal photoreceptors, the cells that turn light entering the eye into electrochemical signals that allow us to see. Once born, these cells must function throughout life. Thus, dysfunction or death of photoreceptors in retinal and macular degenerative diseases causes irreversible vision loss.

Multiple planes of the retina visualized through Optical Coherence Tomography
Winnette McIntosh Ambrose, Ph.D., a postdoctoral fellow in the lab, had begun exploring the use of biomaterials for growing photoreceptor cells. Photoreceptors in cell culture and other artificial systems, however, fail to form normally in the absence of the retinal pigment epithelium (RPE). In the eye, the RPE serves as a barrier between the blood and the neural network of the retina, providing nutrients and removing debris. Fortunately, Ambrose and Swaroop had the expertise at hand to tackle this challenge.

Dr. Swaroop and his laboratory
“Several months ago, Dr. Enrique Rodriguez-Boulan came to do a sabbatical in our laboratory,” Swaroop says. Rodriguez-Boulan, Ph.D., a Professor at Cornell Medical School in New York, studies the cellular polarity of retinal pigment epithelium (RPE). “We created a very elaborate project to do a three-dimensional reconstruction of the outer retina which includes both RPE and photoreceptors.”
Their goal is to create a model system that can be used not only to study basic biology and screen for small molecules drugs, but ultimately for transplantation. They plan to embed photoreceptor precursor cells in a biomaterial that will direct structured growth and integration with RPE cells growing in culture or on a matrix.
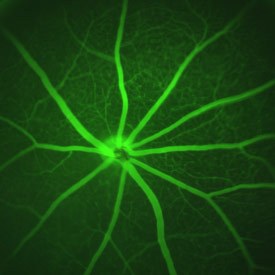
Vasculature of the retina
The project involves what Swaroop describes a “United Nations” of scientists with widely differing expertise. Other members of his team at NIH include a newly recruited Japanese physiologist, Kohei Homma, Ph.D., and a Taiwanese ophthalmologist, Yi-Sheng Chang, M.D. And to kick off the effort, on March 2, 2011, Swaroop convened a meeting of experts in bioprinting, nanomaterials, and imaging from industry and academia to make sure their team has considered all the angles and help to chart a course of action.
“As a Branch Chief, I need only think of the big-picture goals, set the directions, find the right people and bring them together to solve problems,” says Swaroop, who moved to the NIH from the University of Michigan in the fall of 2007.
Swaroop is not short of ambitious goals. Finding and purifying the right precursor cells in sufficient quantities is a challenge for any cell-based therapy and photoreceptors are no exception. In a pool of 100,000 neuronal cells derived from stem cells, only five to twenty percent are the photoreceptor cells that matter. “A few years ago, in a paper in Nature, we showed that cell-based retinal therapies are possible,” said Swaroop. “But one problem is to purify the photoreceptor precursors; we don’t have cell surface markers to identify them.”
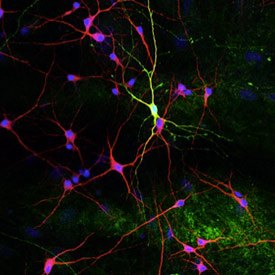
Neurons in culture
Thus, Swaroop’s laboratory is attempting to map regulatory networks that guide photoreceptor development by simultaneously introducing multiple “reporters” of gene expression into stem cells and following these markers as the cells differentiate and specialize. In this way, Swaroop and his team can determine which markers define the cells that ultimately become photoreceptors. Although such an approach sounds straightforward, the technical challenges of introducing multiple reporters are large. “Its cumbersome, time consuming, and expensive work,” said Swaroop. “But the use of cell therapies will never be approved until you can safely define the whole population of cells you are working with.”
Anand Swaroop, Ph.D., is Chief of the Neurobiology Neurodegeneration & Repair Laboratory at the National Eye Institute (NEI).
This page was last updated on Wednesday, May 24, 2023