The Human Energy Crisis
Kevin Hall applies a physicist’s view of energy to the human body.
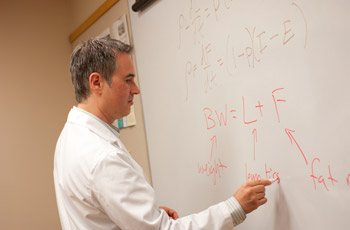
Kevin Hall, Ph.D., designs mathematical tools that help overweight people shed pounds and keep them off
With more than one-third of adults in the U.S. now considered obese, research into how food choices affect metabolism has become a public health priority. Leading the way, and overturning conventional weight-loss myths in the process, is Kevin Hall, Ph.D., a physicist with an uncommonly mathematical approach to the science of energy expenditure.
Guiding an expert team of mathematicians, neuroscientists, and dieticians, Hall’s lab broke new ground by modeling the dynamics of energy expenditure and body composition when people alter their diets and physical activity, while collaborating with clinicians at the NIH Clinical Center to test their models’ predictive abilities in real people under strict experimental control.

Team members (l to r) Arjun Sanghvi, Kevin Hall, Stephanie Goodwin, and Juen Guo review progress on new metabolic models
“My background is in physics, so obesity is not my initial area of research,” Hall says. “When I first came to the NIH in 2003, I was fascinated to learn about the various measurements that would be possible in our Metabolic Research Unit, which was then just finishing construction.”
For decades, dieters were told that reducing their cumulative food consumption by 3,500 calories would result in a one-pound loss of weight, based on the amount of energy stored within that pound of human fat tissue. But, much to the frustration of dieters, Hall found the estimate to be overly optimistic because it does not account for metabolic changes during dieting and weight loss.

Amanda, a research participant, talks with Senior Investigator Kevin Hall (center) and Staff Clinician Bernard Miller about plans for her two-week stay at the NIH Clinical Center
To design more advanced algorithms, Hall and his colleagues mined information from well-controlled metabolic research studies throughout history and from all over the world. Some of their sources are surprising, including data from starvation studies in professional hunger artists of the nineteenth century.
Hall’s team then developed the Body Weight Simulator to more accurately predict the lifestyle changes needed to reach and maintain a particular weight goal. Thus far, almost a million people have used the tool. Recently, Hall and colleagues extended the model to account for growth and development in children and adolescents. The model for kids showed that they require many more excess calories per pound of excess weight gain compared to adults.

Postdoctoral Fellow Stephanie Goodwin (right) and Postbaccalaureate Fellow Thomas Bemis prepare to measure a research participant’s resting energy expenditure with a ventilated hood
In addition, Hall recognized the need for a more physiological understanding of metabolism that accounts for diet composition, not just calories. So the team created a detailed model of carbohydrate, fat, and protein metabolism.
“The human body is like a ‘flex-fuel’ car engine: you can throw in diesel one day, regular gas the next day, ethanol the day after,” Hall explains. “But the body is even more complex, because there is no fuel tank—we are built out of fuel, with each cell a miniature engine constantly turning over its components and all functioning surprisingly well despite enormous variations in diet.”

A research participant prepares for a 24-hour stay in one of the NIH Clinical Center’s metabolic chambers, allowing extremely accurate metabolism measurements
Ultimately, the test of any model is whether it can predict the outcome of a future experiment, so Hall leads a clinical study to compare the ever-popular low-carb diet with a standard low-fat diet in a controlled in-patient setting. Hosting research participants in the NIH Clinical Center’s Metabolic Research Unit for two weeks at a time, Hall asks, “If we cut carbs versus cutting fat, in the same people, what happens to metabolic fuel consumption, and which diet leads to more body fat loss?” The study is ongoing, but preliminary data appear to validate the model predictions.
The models don’t yet address how we decide when, where, what, and how much to eat. Since dynamic interactions between homeostatic, hedonic, and cognitive processes determine eating behavior, Hall’s team collaborated with the National Institute of Mental Health (NIMH) to perform brain scans of trial participants.
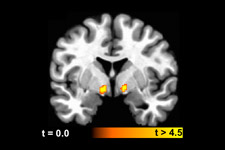
An fMRI image shows the correlation between increased activity in the ventral pallidum region of the brain and the research subjects’ ratings of how pleasant it would be to eat a variety of foods
“Food stimulates the brain’s reward circuitry during both anticipation and consumption, so we wanted to know what happens in the brains of our study subjects when exposed to food cues and how this changes when they are placed on low-fat or low-carb diets,” Hall says.

Dr. Hall and Staff Scientist Juen Guo (right) analyze brain reward circuitry by measuring dopamine receptor binding potential
Using functional magnetic resonance imaging (fMRI), the team examined brain activity in response to viewing and ingesting various foods. They identified the brain regions associated with inferring how pleasant it would be to eat foods based only on visual cues. Hall believes this finding is particularly important in light of the ubiquity of food images in TV shows and advertisements that are meant to entice us to eat.
“It’s really exciting to work with this diverse group of people attacking the same set of problems from very different perspectives,” Hall says.
Kevin Hall, Ph.D., is a Senior Investigator in the Laboratory of Biological Modeling at the National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK).
Further reading:
This page was last updated on Monday, April 21, 2025