Blood Test May Point to Timing of Breast-Cancer Diagnosis
Shifts in White Blood-Cell Types Leading Up to a Breast-Cancer Diagnosis
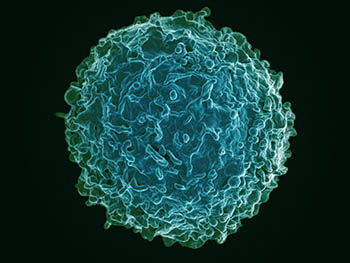
CREDIT: NIAID
Colorized scanning electron micrograph of a B cell from a human donor. The profile of B cells and other white blood cells in a woman’s bloodstream may indicate future risk of developing breast cancer.
Shifts in the populations of different types of leukocytes, or white-blood cells, in a woman’s bloodstream may signal a later diagnosis of breast cancer according to a study by researchers at the National Institute of Environmental Health Sciences (NIEHS). The scientists found that women with higher proportions of B cells experienced a higher risk of breast cancer years later. It also found that women with lower concentrations of monocytes had a higher risk for developing breast cancer in the near term.

Jack Taylor
“This finding opens up a new avenue for looking at breast-cancer risk,” said senior study author Jack Taylor, head of the NIEHS Molecular and Genetic Epidemiology Group. “Although we know a lot about how the immune system interacts with a tumor, this is one of the first studies to detail changes in circulating immune cells in the months and years before diagnosis.”
Refining risk
The new study is one of a slew of recent findings to emerge from the Sister Study, an NIEHS research initiative that enrolled women who have a biological sister with breast cancer but did not have the disease themselves.

Jacob Kresovich
Jacob Kresovich, a postdoctoral fellow in Taylor’s lab, said previous research indicated that women with higher numbers of total white blood cells may be at higher risk of breast cancer. “But white blood cells are really diverse and can be further classified based on their subtype and overall function,” said Kresovich, who is lead author of the paper. “We believed we could refine some of these associations by looking at the relationship between specific types of cells and the incidence of breast cancer.”
Timing is everything
From 53,000 women enrolled in the Sister Study, the researchers selected 2,774 participants to include in this analysis. They used a sophisticated technique called methylation cytometry to estimate the proportions of six different subtypes of white blood cells in each of the women’s blood samples.
The researchers found that the composition of white-blood-cell subtypes changed in the years leading up to a breast-cancer diagnosis. The proportion of monocytes, a type of white blood cell that can be activated in the presence of growing tumors, decreased in the bloodstream of women who were diagnosed with breast cancer in the year after blood draw. “Monocytes may be recruited to cancer tissue, which would explain why there would be a drop in blood shortly before the diagnosis of cancer,” said Kresovich.
In contrast, the proportion of B cells, which produce antibodies to fight infection and disease, was higher in women who were diagnosed four or more years later. Taylor said although the shift in the profile of these cells seems to be associated with tumors arising in the distant future, this finding needs confirmation.
“Next, we want to look more broadly at the information we can extract from these profiles and improve our predictions of who will develop cancer,” said Taylor. “We would also like to understand whether certain health behaviors alter these profiles.” (NIH authors: J.K. Kresovich, K.M. O’Brien, Z. Xu, C.R. Weinberg, D.P. Sandler, and J.A. Taylor; JAMA Netw Open 3:e1919536, 2020; DOI:10.1001/jamanetworkopen.2019.19536)
Adapted from an article that appeared in the February 2020 issue of the NIEHS Environmental Factor.
This page was last updated on Tuesday, March 29, 2022
